Generally speaking, everything that enters your body through your digestive system must be excreted back into the environment in some form eventually. Most of the waste products of cellular metabolism and many other substances exit your body via your urinary system. Urine is the body’s primary waste product, and urination (the release of urine to the environment) is the final step of metabolism.
In this chapter, we take you on a tour of the urinary system, reveal the makeup of urine, and explain how the kidneys help your body maintain homeostasis.
Running Down the Urinary System's Responsibilities
The functions of the human urinary system, as defined in the following list, are similar to those of typical reptiles, birds, and mammals, with some differences in the details.
● Doing the dirty work: Cellular metabolic wastes are toxic and would cause harm to the cell if they were allowed to accumulate. Cells, therefore, continuously export their metabolic wastes into the extracellular fluid. As extracellular fluid is absorbed into the venous blood during capillary exchange, the waste substances enter the circulatory system. Carbon dioxide is excreted in the lungs in the pulmonary circulation cycle. Other byproducts of cellular metabolism travel in the arterial (oxygenated) blood to the renal artery and into the kidney. The function of the urinary system is to remove these toxic byproducts from the blood and then eliminate them from the body.
The term excretion can mean the movement of material from the inside to the outside of a cell, as well as the release of material from the inside to the outside of the body.
● Making and expelling urine: Urine is a watery solution produced by your kidneys. It's the matrix through which the water-soluble waste products of metabolism, mainly nitrogenous metabolic byproducts, are removed from the blood and eliminated from the body. Urine also helps maintain the chemical equilibrium of the blood because substances harmful to the chemical equilibrium of the blood can be dumped there.
● Balancing water content: Around half of your body weight is water, contained in intracellular and extracellular fluid, the plasma of your blood, your lymph fluid, and the fluids in your digestive tract and mucous membranes. Your kidneys precisely regulate the release and retention of water to maintain blood volume, composition, and chemical variables within homeostatic ranges.
● Performing endocrine functions: The kidney is one of the most important endocrine organs. The adrenal endocrine glands are located on top of the kidneys but outside the kidney capsule, so they're not part of the kidneys. Many of the hormones produced and secreted by these glands act on the kidneys.
• Regulating RBC production: The hormone erythropoietin, which regulates RBC (red blood cell) production (erythropoiesis) in the bone marrow, is produced in the peritubular capillary endothelial cells in the kidney and liver. Erythropoietin also has other physiological functions related to wound healing and recovery.
• Regulating bone growth: Calcitriol, the physiologically active form of vitamin D, is synthesized in the kidneys from a precursor molecule synthesized in the liver. Calcitriol regulates, among other things, the concentration of calcium and phosphate in the blood, which promotes the healthy mineralization, growth, and remodeling of bone.
Surveying the Structures of the Urinary System
The human urinary system is quite compact. Unlike some other organ systems, you can identify the point where it begins and another point, not too far away, where it ends.
Like the alimentary canal, the urinary system is essentially a system of tubes through which a substance passes, undergo - ing a series of physiological processes as it does so. The familiar tissue layers — an outer fibrous covering, a muscular layer, and a mucous layer lining the interior surface — are seen throughout the urinary system, beginning at the ureter. The mucus protects the tissues from the caustic urine.
The following sections get you acquainted with the various parts of the urinary system.
Creating urine: The kidneys
The urinary system begins with the kidneys, fist-sized paired organs that are reddish-brown in color and located just below the ribs in your lower back. A single kidney is shaped like an elongated oval; actually, it’s shaped just like a kidney bean. (Coincidence?) The inner curve of the kidney has a large concavity (depression) called the hilum where a number of vessels enter or exit, including the ureter, renal artery, renal vein, lymphatic vessels, and nerves. A connective tissue membrane called the peritoneum, as well as adipose (fat) tissue, attach your kidneys to your posterior abdominal wall. (The term renal comes from the Latin ren, meaning “kidney.”)
Beneath the peritoneum, a lining of collagen called the capsule encloses the kidney. Fibers of this layer extend outward to attach the organ to surrounding structures.
Renal blood supply
The renal artery, a large branch of the abdominal aorta, brings blood into the kidney for filtering. The renal vein drains filtered blood out of the kidney. The kidneys receive about 20 percent of all blood pumped by the heart each minute.
Kidney tissues
Under the capsule, the kidney’s various tissues are arranged in more or less concentric layers. The outermost layer, just beneath the capsule, is the cortex. Beneath the cortex is the medulla, a series of fan-shaped structures comprising a membrane that’s convoluted (folded) into conical structures, called renal pyramids, that secrete urine at their tips into sac-like structures. The innermost layer is the renal pelvis, which channels the urine from these sacs into the ureter.
Nephron
Microscopic in size (about a million of them exist in each kidney), the nephron is the kidney’s filtering unit. Each nephron has two parts: the renal corpuscle and the renal tubule. The renal corpuscle also has two parts: the glomulerus (plural, glomeruli), a special kind of capillary bed derived from arterioles branching from the renal artery, and the glomerular capsule or Bowman’s capsule, a doublewalled epithelial cup that partially encloses the glomerulus.
Leading away from the capsule, the nephron loops up, forming the proximal convoluted tubule, or PCT. The tube then straightens, pushing down into the medulla and looping up again (the loop of Henle). At the top, it loops again into the distal convoluted tubule (DCT). This tubule connects with a collecting duct that carries the urine through the renal pyramids into a series of sac-like structures in the renal pelvis.
The nephrons are surrounded by the peritubular capillaries, which perform an important role in direct secretion, selective reabsorption, and the regulation of water.
Make sure you keep the kidney capsule and the glomerular capsules straight. The kidney has one kidney capsule on the outside and a million microscopic glomerular capsules inside.
Holding and releasing: The urinary tract
All complex animals have evolved ways of removing metabolic waste and regulating water balance, but only mammals have evolved an organ, the bladder, for sequestering urine so it may be excreted voluntarily. Whatever the evolutionary imperative that caused the development of this part of the mammalian urinary system, some groups have developed chemical signaling mechanisms that utilize it. For humans, the ability to control the time and place of urination may be crucial for their ability to live in dense groups.
The urinary tract is the name of the part of the urinary system from the top of the ureter to the external urethral opening, the route of urine out of the body. It consists of the ureters, bladder, and urethra.
Ureters
The ureters are tubes that transport urine from a kidney to the bladder. The ureter emerges from the renal pelvis.
The walls of the ureter are similar in structure to those of the intestines: The muscular layer contracts in waves of peristalsis to move urine from the kidney to the bladder.
Bladder
The bladder is a hollow, funnel-shaped sac into which urine flows from the kidneys through the ureters. The bladder has a capacity of about 20 ounces (about three-fifths of a liter). It lies in the pelvic cavity, just behind the pubic bones and centered in front of the rectum. In females, it’s in front of the uterus and vagina.
Like other organs in the urinary and digestive systems, the bladder is made up of an outer protective membrane, several layers of muscles arranged in opposing directions, and an inner mucosal layer. The muscle layers contract to expel urine into the urethra. The mucosa is made up of a special kind of epithelial tissue called transitional epithelium in which the cells can change shape from columnar to squamous to accommodate larger volumes of urine (see Figure 7-1). Pressure (stretch) receptors in the muscle layer send impulses to the brain when the bladder is becoming full.
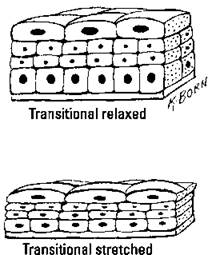
Figure 7-1: Transitional epithelium lines the bladder.
Urethra
The urethra is a tube that carries urine from the bladder to an opening (orifice) of the body for elimination. The mucosa (epithelium) of the urethra is composed of transitional cells as it exits the bladder. Farther along are stratified columnar cells, followed by stratified squamous cells near the external urethral orifice. Mucus from small glands in the mucosa help protect the epithelium from the corrosive urine.
In both males and females, a sphincter at the proximal end of the urethra (between the bladder and the urethra) retains urine in the bladder. This sphincter, called the internal urethral sphincter, is made of smooth muscle and is under the control of the autonomic nervous system. It opens to release urine into the urethra.
Where the urethra traverses the urogenital diaphragm (the floor of the pelvis), there’s a sphincter made of striated fibers (skeletal muscle) called the external urethral sphincter, which is under voluntary control.
The male and female urethrae are adapted to interact with the respective reproductive systems (which we cover in Chapter 8) and, therefore, differ from each other in some aspects of anatomy and physiology.
● Female urethra: In females, the urethra is about 1.5 inches (3.8 centimeters) long, from its point of emergence from the bladder to the urethral orifice. It runs along the anterior wall of the vagina and opens between the clitoris and the vaginal orifice. The external sphincter is located just inside the exit point.
● Male urethra: In males, the urethra is about 8 inches (20 centimeters) long, from its point of emergence from the bladder to its opening at the tip of the penis, called the urethral meatus. As it passes through the prostate gland and the penis, the male urethra is divided into three named sections, based on anatomical structures:
• The prostatic urethra contains the internal sphincter and passes through the prostate. Openings in this region allow for the passage of sperm and prostatic fluid into the urethra during orgasm.
• The membranous urethra contains the external sphincter. It's only about 1 inch (2.5 centimeters) in length.
• The cavernous urethra, or spongy urethra, runs the length of the penis on its ventral surface, ending at the urethral meatus.
The Yellow River
Urine is a bodily fluid with specific functions, just like blood and lymph. But unlike those, you see urine in the normal course of everyday events. Here’s everything you always wanted to know about how it gets to be its own sweet self.
Looking at the composition of urine
Urine is about 95 percent water, in which is dissolved urea, other nitrogenous compounds, and varying concentrations of electrolytes, plus assorted inorganic and organic compounds. Its odor comes from ammonia and other substances derived from ammonia, such as urea. See Table 7-1 for more about the nitrogenous components of urine.
Table 7-і Nitrogenous Components of Urine and Their Sources
|
Nitrogenous Component |
Source |
|
Urea |
A byproduct of the breakdown of amino acids |
|
Creatinine |
A byproduct of the metabolism of the amino acid |
|
creatine, present in large quantities in muscle cells |
|
|
Ammonia |
A byproduct of the breakdown of proteins |
|
by bacteria |
|
|
Uric acid |
A byproduct of the breakdown of nucleotides |
Urine is yellow because it contains urobilinogen, a compound formed from the breakdown of red blood cells. The normal color range of urine is some shade of yellow, from nearly clear to dark amber, depending mostly on one’s level of hydration. When you’re abundantly hydrated, lots of water goes into the urine, making it more diluted and, therefore, paler. When you’re less than optimally hydrated, the kidneys put less water into the urine. As a result, the urine becomes more concentrated and appears darker.
Ingested food, beverages, and pharmaceutical products influence the composition of urine. Urine contains hippuric acid, produced by the digestion of fruits and vegetables, and ketone bodies, produced by the digestion of fats. Some foods, beverages, and drugs impart color and odor to urine. Some physiological conditions and disorders affect the composition of urine, and urine has long been analyzed for clinical signs.
To maintain the blood pH within the homeostatic range (7.3 to 7.4), the kidney can produce urine with a pH as low as 4.5 or as high as 8.5.
Filtering the blood
The glomerulus and the glomerular capsule make up the area of interface between the circulatory system and the kidney. That’s where your body filters blood.
The blood pressure in these capillaries is higher than in other capillaries, and it pushes the blood up against the glomerular wall with some force. Because it’s a process that relies on mechanical force (fluid pressure), glomerular filtration separates particles based on one criterion: molecule size.
The thin, permeable glomerular wall acts as a filtration membrane. Water passes through into the capsule, bringing along small-molecule solutes, including wastes and toxins like urea and creatinine and useful small-molecule substances such as glucose, amino acids, and electrolyte ions. Large solutes, such as proteins and nutrients, remain in the plasma inside the glomerular vessel and continue on in the circulating blood. The watery solution (filtrate) passes into the top of the renal tubule at the capsule.
Reabsorbing selectively
An important aspect of urine production is the restoration of glucose, amino acids, and electrolyte ions, not to mention water, from the filtrate to the blood. As the filtrate passes along the nephron, it’s acted upon by different types of specialized tissue. Processes in the following specialized tissues are responsible for the composition of urine:
● Microvilli: Microvilli line the nephrons, increasing the surface area within the tubule where substances can enter and leave the filtrate.
● PCT: Na+ (sodium ion) undergoes active transport from the filtrate to the blood at the PCT. Where Na+ goes, Cl- just naturally follows. This situation creates an osmotic pressure gradient that pulls water out of the filtrate and into the blood. Approximately 65 percent of the water and salts are returned to the blood at the PCT.
Some substances, including K+ and some hormones, are secreted from the adjacent peritubular capillaries into the PCT. This process is termed direct secretion.
● Loop of Henle: At the loop of Henle, electrolytes and urea move out of the nephron into the medulla. The filtrate remaining in the nephron, now urine, drains through the DCT into the collecting duct and then into the renal pelvis.
● Medulla: The solutes that enter the medulla from the loop of Henle draw water into the medulla. Capillaries in the medulla restore some of the water to the blood.
● DCT: Active transport passes amino acids, glucose, and electrolytes (those useful substances that happen to be small enough to pass through the filtration membrane) back into the blood at the DCT. Water reabsorption at the DCT occurs under the control of ADH.
● Collecting duct: Reabsorption of water occurs in the collecting duct. As salts are reabsorbed, water follows. The amount of water reabsorbed from the filtrate back into the blood depends on the hydration situation in the body. However, even in cases of extreme dehydration, the kidneys produce around 16 ounces (about half a liter) of urine per day just to excrete toxic waste substances.
Numerous other substances are returned to the blood at specific points, conserving them and maintaining the blood's chemical environment. More than 99 percent of the filtrate produced each day can be reabsorbed. The processes are called selective reabsorption because the details are different for (chemically) different types of substances.
Expelling urine
Urine drips down the nephron’s collecting ducts to the renal pelvis. From there, it moves along the ureter and into the bladder. As the urine accumulates, the pressure receptors in the lining send signals to the brain. The first message is sent when the bladder is about half full (around 6 to 8 ounces, or 177 to 237 milliliters). At a volume of 12 ounces (354 milliliters), the messages become stronger, and it becomes difficult to control the external urethral sphincter.
When the time is right to empty the bladder, the brain sends an impulse through the autonomic nervous system to open the internal urethral sphincter and contract the bladder muscles. Urine flows out of the bladder, through the urethra, and out of the body.
Maintaining Homeostasis
The chemistry of life, stunningly complex and precise, requires a tightly controlled environment to proceed optimally. The kidneys, under hormonal control, are key organs for maintaining the chemical homeostasis of blood and other body fluids. The endocrine system has a huge range of subtle and interacting mechanisms for controlling kidney function. (See Chapter 9 for the scoop on the endocrine system.)
Connecting fluid balance and blood pressure
Aspects of fluid balance that involve the blood include blood volume and the amount and nature of the electrolytes in the plasma. These factors are linked, as we explain in the following sections.
Blood volume (water content)
The concentration of electrolytes (ions), such as Na+, Cl-, and K+, helps determine overall blood volume because the kidneys push water into the blood or withdraw water from the blood to bring the concentrations of these electrolytes within homeostatic ranges.
Blood volume is an important factor in circulation. For values above the optimum range, the greater the blood volume, the harder the heart must work to pump the blood, and the greater the fluid pressure in the arteries. For values below the optimum range, the less the blood volume, and the weaker the pressure filtration in the glomeruli (as well as the effects of inadequate circulation in all tissues and organs). However, the urinary system, when functioning properly, maintains blood chemistry (electrolyte concentration in the plasma), even if that requires putting some strain on other systems.
Hormonal mechanisms to control blood volume
The renin-angiotensin system (RAS) (also called the renin- angiotensin-aldosterone system [RAAS]) is called into action when the presence of toxins in the blood signals low blood pressure in the glomeruli. Specialized kidney cells secrete the enzyme renin, also called angtiotensinogenase, which sets off a series of reactions in different organ systems, eventually resulting in the production of the hormone angiotensin II, a powerful vasoconstrictor. Angiotensin II also stimulates the secretion of the hormone aldosterone from the adrenal cortex, which causes Na+ to be reabsorbed from the nephrons into the blood. Where salt goes, water follows. The movement of water into the blood increases blood volume, which, along with the vasoconstriction, raises blood pressure and enhances the effectiveness of the glomerular filtration.
The pituitary gland secretes ADH when the hypothalamus senses dehydration (from a lack of water consumption or a loss of water through sweating, diarrhea, or vomiting). Sodium is reabsorbed by the nephrons but not enough water follows, so ADH causes more water to be reabsorbed from the urine, which decreases the amount of urine and helps maintain normal blood volume and pressure.
Atrial natriuretic hormone (ANH) is a polypeptide hormone secreted by heart muscle cells in response to signals from sensory cells in the atria that blood volume is too high. ANH prevents the kidneys from secreting renin. In fact, the overall effect of ANH is to counter the effects of the RAS. ANH acts to reduce the water, sodium, and adipose (fat molecules) loads on the circulatory system, thereby reducing blood pressure.
Regulating blood pH
The homeostatic range for blood pH is narrow. The optimum value is around 7.4 (slightly alkaline). Alkalosis (increase in alkalinity) is life-threatening at 7.8. Acidosis (increased acidity) is life-threatening at 7.0.
Neutral pH is 7.0, the value for water.
Acids and, to a lesser extent, alkalis (bases) are products or byproducts of metabolic processes. The digestion of fats produces fatty acids. Capillary exchange acidifies the blood because the metabolic waste carbon dioxide is combined with water in the red blood cells, forming carbonic acid. Muscle activity produces lactic acid. Some acids are ingested in food and drink. The kidneys respond to changes in blood pH by excreting acidic or basic ions into the urine.
Your body has buffering processes in which the kidneys are involved. A buffer is a type of chemical that binds with either acid or base as needed to increase or decrease the solution pH. Buffers are made in cells and available in the blood.
Three mechanisms work together to maintain tight control over blood pH:
● Minor fluctuations in pH are evened out by the mild buffering effects of substances always present in the blood, such as the plasma proteins.
● When sensors in the kidneys detect that the blood is too acidic, they induce the breakdown of the amino acid glutamine, releasing ammonia, a basic substance, into the blood. When the ammonia arrives at the kidney, it's exchanged for Na+ in the urine and eliminated.
● By far the most important buffer for maintaining acid-base balance in the blood is the carbonic-acid-bicarbonate buffer.
The body maintains the buffer by eliminating either the acid (carbonic acid) or the base (hydrogen carbonate ions). Carbonic acid concentration can be reduced within seconds through increasing respiration — the excretion of carbon dioxide through the lungs increases pH. Hydrogen carbonate ions must be eliminated through the kidneys, a process that takes hours.