A Breath of Fresh Air
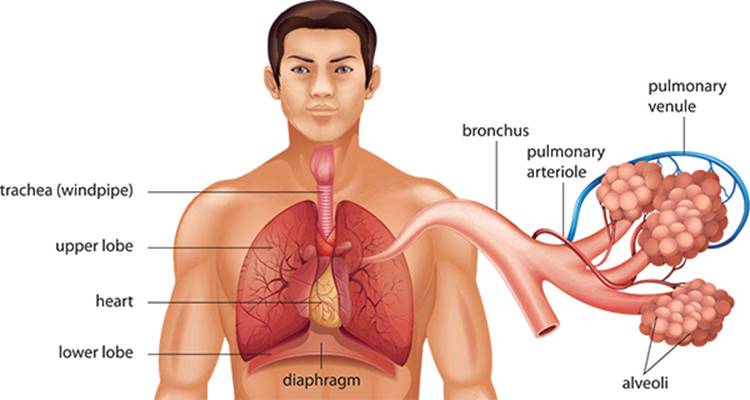
RESPIRATORY SYSTEM
The role of the respiratory system is rather simple: bring oxygen (O2) to the tissues and remove carbon dioxide (CO2) from the body. This system is divided into the conduction zone, where the air is transported but gases are not exchanged with the blood, and the respiratory zone, where gases are passed between the airways and the blood.
Respiratory Epithelium
The lining of the respiratory tract warms, humidifies, and cleans the air as it passes down the tract before entering the lungs. Specialized cells facilitate these functions. In the respiratory tract, the epithelium is arranged into respiratory mucosa, a collection of cells that give the appearance of being multilayered. However, every cell has an attachment to the basement membrane. Every cell does not, however, reach the lumen, which results in nuclei being at different levels—an example of a pseudostratified columnar epithelium.
Columnar Epithelium
The surface epithelial cells are taller than they are wide, so they are columnar in appearance. This shape is simply due to their arrangement in the layer and does not have a practical significance otherwise. However, modifications to their apical (facing the lumen or surface) membranes play a crucial role for the respiratory system.
Extensions of the cell membrane are projected into the lumen as cilia. They have a core of microtubules (a cytoskeletal polymer) that are anchored to the cytoskeleton at the base (basal body) and freely extend outward as the main body or shaft of the cilia.
What is the difference between cilia and hair?
Cilia are often compared to hairs, but are completely different in molecular organization and scale (hairs are made up of cells and cilia occur on single cells in the hundreds).
Using the microtubule associated proteins (MAPs), dynein and nexin, the core of the microtubules can be made to slide relative to each other and results in bending of the cilia. When the dynein completes the bending cycle, which requires ATP, the resulting relaxation and rebound is created by nexin, which is rather elastic in nature. This active bending and rebounding causes the cilia to wave back and forth and creates a current that is capable of moving surface material. When working in concert, all the cilia on all the columnar cells of the respiratory tract can beat to move material up and out of the respiratory tract. A sticky material that traps the particulate material aids this movement. It can then be more efficiently transported.
Goblet Cells
These are the same cells as are found in the digestive tract, which produce a thick, sticky mucus. In the respiratory system, the mucus acts as a dust trap to grab particles from the air so they can be more efficiently transported upward and eventually out of the respiratory tract.
Nose
The nasal cavity is one of the two ways air can enter the body, the other being the mouth. Air passes through the nostrils (external nares) and, because of the nasal septum, remains either on the right or left side. Once in the cavities themselves, the air first encounters the respiratory epithelium, where it begins the process of being cleared of particulates. Additionally, the air is warmed and humidified. To ensure maximum efficiency in all of these processes, the walls of the nasal cavity have several large folds that project outward into the nasal cavity and expand the surface area where air can be processed before moving farther along the respiratory pathway.
The air then moves toward the back of the nasal cavity and through narrow passages (internal nares) that lead to the top portion of the throat (pharynx). This nasopharynx connects the nasal cavities to the oropharynx, the back of the oral cavity.
Pharynx and Larynx
Commonly referred to as the throat and voice box, the pharynx and larynx respectively mark the beginnings of the respiratory tract and prevent the aspiration of liquid and solid material into the airways. This area also includes the structures essential for vocalization (sound).
Air from the nasopharynx and/or the oropharynx moves downward to the laryngopharynx. This chamber is protected from liquid and particulate matter by the epiglottis. Air easily finds its way around the epiglottis and moves into the larynx.
Within the larynx, connective tissue shelves on the lateral portions of the passageway and muscles create the adjustable cords that vibrate as air moves between them, creating sound. The most superior folds (shelves or chords) are thicker and more substantial in structure to provide a protective umbrella for the more delicate chords that are inferior. These are called the vestibular folds and they protect the vocal folds (vocal chords).
It is these delicate, thin connective tissue shelves that stretch across the laryngeal opening and become taut or loose to provide a larger or smaller opening, which changes the pitch of the sound emanating from the vibrating chords. The vocalis muscle, which is lateral to the folds in this region, directs this tension on the chords.
Trachea and Bronchial Tree
The trachea (commonly called the windpipe) marks the single passage for all air to get to and from the lungs. It lies just under the esophagus and branches off a number of times, some outside but most inside of the lung tissue itself. With each branch, the passageway becomes considerably narrower and the walls of the tubes become thinner until a dead end is reached and gases can be exchanged between the air and the blood.
The trachea is formed with intermittent cartilaginous rings that occur along its length. These incomplete, C-shaped rings provide support for the trachea, especially when you inhale, where the lower pressure would likely cause a less well-supported tube to collapse inward on itself.
The first branching of the bronchiolar tree (the branched air passages) is outside of the lung tissue (extrapulmonary). This splitting up results in a right and a left primary bronchus (plural: bronchi). Because the right lung has three lobes and the left lung has two, greater airflow is needed on the right side, so the right bronchus is larger in diameter than the left.
Primary bronchi divide and give rise to secondary bronchi within the lung tissue, marking the first intrapulmonary bronchi. The right bronchus divides into three secondary bronchi, each going to one lobe in the right lung, and the left bifurcates into two secondary bronchi for each of the lobes of the left lung.
Tertiary bronchi are the next branches that occur on the tree and provide air to a discrete and isolated section of the lung tissue called a bronchopulmonary segment. Connective tissue septa separate these regions from other segments of the lungs. They are completely independent with their own vascular supply and airway. On the right side, there are 10 segments divided unequally between the lobes of the lungs, and eight segments on the left with each lobe divided into four segments each.
These three levels of bronchi end in the next order of branching where the passageways become bronchioles. Bronchioles are much smaller in diameter than bronchi and lack the cartilaginous rings or plates of the bronchi. Layers of smooth muscle wrap around the increasingly smaller-diameter bronchioles to enable them to constrict or dilate as dictated by the autonomic nervous system. From the tertiary bronchi, there are approximately seventeen orders of branching continuing until the end of the conduction zone (the area in which air is passed through the body) is reached and the respiratory zone (where gas exchange occurs) begins.
The terminal bronchiole marks the last segment of the conduction zone (hence the name terminal). The diameters of these passageways are very thin with only one layer or two of smooth muscle present.
Lungs
The tissue that makes up these essential organs is more empty space than actual structure. Take away the bronchiolar tree, blood vessels, and nerves and what remains very much resembles an extremely porous sponge. This thin-walled and porous area marks the bulk of the respiratory zone, where gases can be exchanged between the air and the blood.
Respiratory Zone
From the terminal bronchioles, air passes to the first portion of the respiratory zone, which are called the respiratory bronchioles. These are often difficult to identify histologically because their structure is the same as the terminal bronchiole with one critical exception: the presence of alveoli. These are millions of small bubbles that mark the end of the respiratory zone for the lungs. Composed of flattened epithelial cells and having a diameter of approximately 0.5 μm (a μm is a micrometer, or one-thousandth of a meter), these structures mark the area of gas exchange.
How many alveoli exist in the lung?
There are 300–500 million alveoli in the lung. Scientists estimate that these millions of alveoli make up approximately 30–50 meters of surface area for gas exchange. This is about the size of a standard tennis court.
Following the respiratory bronchioles, the air moves into an alveolar duct. These thin-walled passages are more defined by the alveoli themselves. However, the openings of the alveoli that protrude from this duct possess a single smooth muscle cell, which creates a cellular sphincter to regulate the air moving into these areas. These are viewed as knobs on the lateral aspect of the alveolar duct.
Finally, air moves into a cluster of alveoli called the alveolar sac, which resembles a cluster of grapes. From the common atrium of the sac, air moves into any of the attached alveoli so that gas can be exchanged. Between adjacent alveoli, a small opening or pore exists to help maintain the air pressure throughout all the alveoli that are part of the alveolar sac. These are identified as alveolar pores or pores of Kohn.