Anthony C. Luke, MD, MPH
C. Benjamin Ma, MD
SPINE PROBLEMS
1. Low Back Pain
ESSENTIALS OF DIAGNOSIS
![]() The cause of back pain may be categorized by pain on flexion versus pain on extension.
The cause of back pain may be categorized by pain on flexion versus pain on extension.
![]() Nerve root impingement is suspected when pain is leg-dominant rather than back-dominant.
Nerve root impingement is suspected when pain is leg-dominant rather than back-dominant.
![]() Alarming signs for serious spinal disease include unexplained weight loss, failure to improve with treatment, severe pain for more than 6 weeks, and night or rest pain.
Alarming signs for serious spinal disease include unexplained weight loss, failure to improve with treatment, severe pain for more than 6 weeks, and night or rest pain.
![]() The cauda equina syndrome often presents with bowel or bladder symptoms (or both) and is an emergency.
The cauda equina syndrome often presents with bowel or bladder symptoms (or both) and is an emergency.
![]() General Considerations
General Considerations
Low back pain is the most common cause of disability for patients under the age of 45 and is the second most common cause for primary care visits. The annual prevalence of low back pain is 15–45%, and the annual cost in the United States is over $50 billion. Approximately 80% of episodes of low back pain resolve within 2 weeks and 90% resolve within 6 weeks. The exact cause of the low back pain is often difficult to diagnose; its cause is often multifactorial, although there are usually degenerative changes in the lumbar spine.
Alarming symptoms for back pain caused by cancer include unexplained weight loss, failure to improve with treatment, pain for more than 6 weeks, and pain at night or rest. History of cancer and age > 50 years are other risk factors for malignancy. Alarming symptoms for infection include fever, rest pain, recent infection (urinary tract infection, cellulitis, pneumonia), or history of immunocompromise or injection drug use. The cauda equina syndromeis suggested by urinary retention or incontinence, saddle anesthesia, decreased anal sphincter tone or fecal incontinence, bilateral lower extremity weakness, and progressive neurologic deficits. Risk factors for back pain due to vertebral fracture include use of corticosteroids, age > 70 years, history of osteoporosis, recent significant trauma, or very severe focal pain. Back pain may also be the presenting symptom in other serious medical problems, including abdominal aortic aneurysm, peptic ulcer disease, kidney stones, or pancreatitis.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
The physical examination is best done with the patient in the standing, sitting, supine, and then prone positions to avoid frequent repositioning of the patient. In the standing position, the patient’s posture can be observed. Commonly encountered spinal asymmetries include scoliosis, thoracic kyphosis, and lumbar hyperlordosis. The active range of motion of the lumbar spine can be assessed. The common directions include flexion, rotation, and extension. The one-leg standing extension test assesses for pain as the patient stands on one leg while extending the spine. A positive test can be caused by pars interarticularis fractures (spondylolysis or spondylolisthesis) or facet joint arthritis, although sensitivity and specificity of the test is limited.
Motor strength, reflexes, and sensation can be tested in the sitting position (Table 10–1). The major muscles in the lower extremities are assessed for weakness by eliciting a resisted isometric contraction for approximately 5 seconds. It is important to compare the strength bilaterally to detect subtle muscle weakness. Similarly, sensory testing to light touch can be checked in specific dermatomes for corresponding nerve root function. Finally, the knee (femoral nerve L2–L4), ankle (deep peroneal nerve L4–L5), and Babinski (sciatic nerve L5–S1) reflexes can be checked with the patient sitting.
Table 10–1. Neurologic testing of lumbosacral nerve disorders.

In the supine position, the hip should be evaluated for range of motion, focusing on internal rotation. The straight leg raise test puts traction and compression forces on the lower lumbar nerve roots (Table 10–2).
Table 10–2. Spine: back examination.

Finally, in the prone position, the clinician can carefully palpate each level of the spine and sacroiliac joints for tenderness. A rectal examination is required if the cauda equina syndrome is suspected. Superficial skin tenderness to a light touch over the lumbar spine, overreaction to maneuvers in the regular back examination, low back pain on axial loading of spine in standing, inconsistency in the straight leg raise test or on the neurologic examination suggest nonorthopedic causes for the pain or malingering.
B. Imaging
In the absence of alarming “red flag” symptoms suggesting infection, malignancy, or cauda equina syndrome, diagnostic imaging, including radiographs, is not typically recommended in the first 6 weeks. The Agency for Healthcare Research and Quality guidelines for obtaining lumbar radiographs are summarized in Table 10–3. If done, radiographs of the lumbar spine should include anteroposterior and lateral views. Oblique views can be useful if the neuroforamina or lesions need to be visualized. MRI is the method of choice in the evaluation of symptoms not responding to conservative treatment or in the presence of red flags of serious conditions.
Table 10–3. AHRQ criteria for lumbar radiographs in patients with acute low back pain.
Possible fracture
Major trauma
Minor trauma in patients > 50 years
Long-term corticosteroid use
Osteoporosis
> 70 years
Possible tumor or infection
> 50 years
< 20 years
History of cancer
Constitutional symptoms
Recent bacterial infection
Injection drug use
Immunosuppression
Supine pain
Nocturnal pain
AHRQ, Agency for Healthcare Research and Quality.
C. Special Tests
Electromyography or nerve conduction studies may be useful in assessing patients with possible nerve root symptoms lasting longer than 6 weeks; back pain may or may not also be present. These tests are usually not necessary if the diagnosis of radiculopathy is clear.
![]() Treatment
Treatment
A. Conservative
Nonpharmacologic treatments are key in the management of low back pain. Education alone improves patient satisfaction with recovery and recurrence. Patients require information and reassurance when diagnostic procedures are not necessary. Discussion must include reviewing safe and effective methods of symptom control as well as how to decrease the risk of recurrence with proper lifting techniques, abdominal wall/core strengthening, weight loss, and smoking cessation. Strengthening and stabilization effectively reduce pain and functional limitation compared with usual care.
Physical therapy exercise programs can be tailored to the patient’s symptoms and pathology. Spinal manipulation has not shown benefits for low back pain; however, the level of evidence is low quality and limited by small sample sizes. Heat and cold treatments have not shown any long-term benefits but may be used for symptomatic treatment. The efficacy of transcutaneous electrical nerve stimulation (TENS), back braces, physical agents, and acupuncture is unproven. Improvements in posture, core stability strengthening, physical conditioning, and modifications of activities to decrease physical strain are keys for ongoing management.
NSAIDs are effective in the early treatment of low back pain. There is limited evidence that muscle relaxants can provide short-term relief; since these medications have addictive potential, they should be used with care. Muscle relaxants are best used if there is true muscle spasm that is painful rather than simply a protective response. Opioids may be necessary to alleviate pain immediately. Treatment of more chronic neuropathic pain with gabapentin and tricyclic antidepressants may be helpful.
B. Surgical
Surgical indications for back surgery include cauda equina syndrome, ongoing morbidity with no response to > 6 months of conservative treatment, cancer, infection, or severe spinal deformity. Prognosis is improved when there is an anatomic lesion that can be corrected and symptoms are neurologic. Spinal surgery has limitations. Patient selection is very important and the specific surgery recommended should have very clear indications. Patients should understand that surgery can improve their pain but is unlikely to cure it. Surgery is not generally indicated for radiographic abnormalities alone when the patient is asymptomatic. Depending on the surgery performed, possible complications include persistent pain; surgical site pain, especially if bone grafting is needed; infection; neurologic damage; nonunion; cutaneous nerve damage; implant failure; deep venous thrombosis; and death.
![]() When to Refer
When to Refer
• Patients with the cauda equina syndrome.
• Patients with cancer, infection, or severe spinal deformity.
• Patients who have not responded to conservative treatment.
2. Spinal Stenosis
ESSENTIALS OF DIAGNOSIS
![]() Pain is usually worse with back extension and relieved by sitting.
Pain is usually worse with back extension and relieved by sitting.
![]() Occurs in older patients.
Occurs in older patients.
![]() May present with neurogenic claudication symptoms with walking.
May present with neurogenic claudication symptoms with walking.
![]() General Considerations
General Considerations
Osteoarthritis in the lumbar spine can cause narrowing of the spinal canal. A large disk herniation can also cause stenosis and compression of neural structures or the spinal artery resulting in “claudication” symptoms with ambulation. The condition usually affects patients aged 50 years or older.
![]() Clinical Findings
Clinical Findings
Patients report pain that worsens with extension. They describe reproducible single or bilateral leg symptoms that are worse after walking several minutes and that are relieved by sitting (termed “neurogenic claudication”). On examination, patients often exhibit limited extension of the lumbar spine, which may reproduce the symptoms radiating down the legs. A thorough neurovascular examination is recommended (Table 10–1).
![]() Treatment
Treatment
Flexion-based exercises as demonstrated by a physical therapist can help relieve symptoms. Epidural or facet joint corticosteroid injections can also reduce pain symptoms. However, patients who received epidural corticosteroids had less improvement at 4 years among all patients with spinal stenosis and were associated with longer duration of surgery and longer hospital stay. Of note, in 2012, there was a fungal meningitis outbreak related to contamination of injectable methylprednisolone prepared in a single compounding pharmacy.
Spinal decompression (widening the spinal canal or laminectomy), nerve root decompression (freeing a single nerve), and spinal fusion (joining the vertebra to eliminate motion and diminish pain from the arthritic joints) have not been shown to be superior to natural history, placebo treatment, or conservative management of degenerative lumbar disk disease (spondylosis). Some evidence suggests that instrumentation (adding surgical hardware to a spinal fusion) leads to a higher fusion rate, but there is no evidence that it makes any difference to clinical outcomes.
![]() When to Refer
When to Refer
• If a patient exhibits radicular or claudication symptoms > 12 weeks.
• MRI or CT confirmation of significant spinal stenosis.
3. Lumbar Disk Herniation
ESSENTIALS OF DIAGNOSIS
![]() Pain with back flexion or prolonged sitting.
Pain with back flexion or prolonged sitting.
![]() Radicular pain with compression of neural structures.
Radicular pain with compression of neural structures.
![]() Lower extremity numbness.
Lower extremity numbness.
![]() Lower extremity weakness.
Lower extremity weakness.
![]() General Considerations
General Considerations
Lumbar disk herniation is usually due to bending or heavy loading (eg, lifting) with the back in flexion, causing herniation or extrusion of disk contents (nucleus pulposus) into the spinal cord area. However, there may not be an inciting incident. Disk herniations usually occur from degenerative disk disease (dessication of the annulus fibrosis) in patients between 30- and 50-years-old. The L5–S1 disk is affected in 90% of cases. Compression of neural structures, such as the sciatic nerve, causes radicular pain. Severe compression of the spinal cord can cause the cauda equina syndrome, a surgical emergency (see above).
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
Discogenic pain typically is localized in the low back at the level of the affected disk and is worse with activity. “Sciatica” causes electric shock-like pain radiating down the posterior aspect of the leg often to below the knee. Symptoms usually worsen with back flexion such as bending or sitting for long periods (eg, driving). A significant disk herniation can cause numbness and weakness, including weakness with plantar flexion of the foot (L5/S1) or dorsiflexion of the toes (L4/L5). The cauda equina syndrome should be ruled out if the patient complains of perianal numbness or bowel or bladder incontinence.
B. Imaging
Plain radiographs are helpful to assess spinal alignment (scoliosis, lordosis), disk space narrowing, and osteoarthritis changes. MRI is the best method to assess the level and morphology of the herniation and is recommended if surgery is planned.
![]() Treatment
Treatment
For an acute exacerbation of pain symptoms, bed rest is appropriate for up to 48 hours. Otherwise, first-line treatments include modified activities; NSAIDs and other analgesics; and physical therapy, including core stabilization and McKenzie exercises. Following nonsurgical treatment for a lumbar disk for over 1 year, the incidence of low back pain recurrence is at least 40% and is predicted by longer time to initial resolution of pain. Epidural and transforaminal corticosteroid injections can be beneficial, especially in relieving acute radicular pain, although the benefit tends to last only 3 months. These injections may be effective in delaying surgery for chronic low back pain. Oral prednisone can reduce inflammation and is useful in reducing symptoms of acute sciatica; the initial dose is approximately 1 mg/kg once daily with tapering doses over 10 days. Co-analgesics for neuropathic pain, such as the calcium channel alpha-2-delta ligands (ie, gabapentin, pregabalin) or tricyclic antidepressants, may be helpful).
A large, ongoing trial has shown that patients who underwent surgery for a lumbar disk herniation achieved greater improvement than conservatively treated patients in all primary and secondary outcomes except return to work status after 4 year follow-up. So far, disk replacement surgery has not shown benefits beyond generally accepted clinically important differences in short-term pain relief, disability, and quality of life compared with spine fusion surgery.
![]() When to Refer
When to Refer
• Cauda equina syndrome.
• Progressive worsening of neurologic symptoms.
• Loss of motor function (sensory losses can be followed in the outpatient clinic).
4. Neck Pain
ESSENTIALS OF DIAGNOSIS
![]() Most chronic neck pain is caused by degenerative joint disease and responds to conservative treatment.
Most chronic neck pain is caused by degenerative joint disease and responds to conservative treatment.
![]() Cervical radiculopathy symptoms can be referred to the shoulder, arm, or upper back.
Cervical radiculopathy symptoms can be referred to the shoulder, arm, or upper back.
![]() Whiplash is the most common type of traumatic injury to the neck.
Whiplash is the most common type of traumatic injury to the neck.
![]() Poor posture is often a factor for persistent neck pain.
Poor posture is often a factor for persistent neck pain.
![]() General Considerations
General Considerations
Most neck pain, especially in older patients, is due to mechanical degeneration involving the cervical disks, facet joints, and ligamentous structures and may occur in the setting of degenerative changes at other sites. Pain can also come from the supporting neck musculature, which often acts to protect the underlying neck structures. Posture is a very important factor, especially in younger patients. Many work-related neck symptoms are due to poor posture and repetitive motions over time. Acute injuries can also occur secondary to trauma. For example, whiplash occurs in 15–40% of motor vehicle accidents, with chronic pain developing in 5–7%. Neck fractures are serious traumatic injuries acutely and can lead to osteoarthritis in the long term. Ultimately, many degenerative conditions of the neck result in cervical canal stenosis or neural foraminal stenosis, sometimes affecting underlying neural structures. Cervical radiculopathy can cause neurologic symptoms in the upper extremities usually deriving from disease of the C5–C7 disks. Patients with neck pain may report associated headaches and shoulder pain. Thoracic outlet syndrome, in which there is mechanical compression of the brachial plexus and neurovascular structures with overhead positioning of the arm, should be considered in the differential diagnosis of neck pain.
Other causes of neck pain include rheumatoid arthritis, fibromyalgia, osteomyelitis, neoplasms, polymyalgia rheumatica, compression fractures, pain referred from visceral structures (eg, angina), and functional disorders. Amyotrophic lateral sclerosis, multiple sclerosis, syringomyelia, spinal cord tumors, and tropical spastic paresis from HTLV-1 infection can mimic myelopathy from cervical arthritis.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
Neck pain may be limited to the posterior region or, depending on the level of the symptomatic joint, may radiate segmentally to the occiput, anterior chest, shoulder girdle, arm, forearm, and hand. It may be intensified by active or passive neck motions. The general distribution of pain and paresthesias corresponds roughly to the involved dermatome in the upper extremity.
The patient’s posture should be assessed, checking for shoulder rolled forward or head forward posture as well as scoliosis in the thoracolumbar spine. Patients with discogenic neck pain often complain of pain with flexion, which causes cervical disks to herniate posteriorly. Extension of the neck usually affects the neural foraminal and facet joints of the neck. Rotation and lateral flexion of the cervical spine should be measured both to the left and the right. Limitation of cervical movements is the most common objective finding.
A detailed neurovascular examination of the upper extremities should be performed, including sensory input to light touch and temperature; motor strength testing, especially the hand intrinsic muscles (thumb extension strength [C6], opponens strength [thumb to pinky] [C7], and finger abductors and adductors strength [C8–T1]); and upper extremity reflexes (biceps, triceps, brachioradialis). True cervical radiculopathy symptoms should match an expected dermatomal or myotomal distribution. The Spurling test involves asking the patient to rotate and extend the neck to one side (Table 10–4). The clinician can apply a gentle axial load to the neck. Reproduction of the cervical radiculopathy symptoms is a positive sign of nerve root compression. Palpation of the neck is best performed with the patient in the supine position where the clinician can palpate each level of the cervical spine with the muscles of the neck relaxed.
Table 10–4. Spine: neck examination.

B. Imaging
Radiographs of the cervical spine can assist in determining the area of degenerative changes. Useful views include the anteroposterior and lateral view of the cervical spine. The odontoid view is usually added to rule out traumatic fractures and congenital abnormalities. Oblique views of the cervical spine can provide further information about arthritis changes and assess the neural foramina for narrowing. Many plain radiographs are completely normal in patients who have suffered an acute cervical strain. Loss of cervical lordosis is often seen but is nonspecific. Comparative reduction in height of the involved disk space and osteophytes are frequent findings when there are degenerative changes in the cervical spine.
CT scanning is the most useful method if bony abnormalities, such as fractures, are suspected. MRI is the best method to assess the cervical spine since the soft tissue structures (such as the disks, spinal cord, and nerve roots) can be evaluated. If the patient has signs of cervical radiculopathy with motor weakness, these more sensitive imaging modalities should be obtained urgently.
![]() Treatment
Treatment
In the absence of trauma or evidence of infection, malignancy, neurologic findings, or systemic inflammation, the patient can be treated conservatively. A course of neck stretching, strengthening and postural exercises in physical therapy have demonstrated benefit in relieving symptoms. A soft cervical collar can be useful for short-term use (up to 1–2 weeks) in acute neck injuries. Chiropractic manual manipulation and mobilization can provide short-term benefit for mechanical neck pain. Although the rate of complications is low (5–10/million manipulations), care should be taken whenever there are neurologic symptoms present. Specific patients may respond to use of home cervical traction. NSAIDs are commonly used and opioids may be needed in cases of severe neck pain. Muscle relaxants (eg, cyclobenzaprine 5–10 mg orally three times daily) can be used short-term if there is muscle spasm or as a sedative to aid in sleeping. Acute radicular symptoms can be treated with neuropathic medications (eg, gabapentin 300–1200 mg orally three times daily), and a short course of oral prednisone (5–10 days) can be considered (starting at 1 mg/kg). Cervical foraminal or facet joint injections can also reduce symptoms. Surgeries are successful in reducing neurologic symptoms in 80–90% of cases but are still considered as treatments of last resort.
![]() When to Refer
When to Refer
• Patients with severe symptoms with motor weakness.
• Surgical decompression surgery if the symptoms are severe and there is identifiable, correctable pathology.
HIP
1. Hip Fractures
ESSENTIALS OF DIAGNOSIS
![]() Internal rotation of the hip is the best provocative diagnostic maneuver.
Internal rotation of the hip is the best provocative diagnostic maneuver.
![]() Hip fractures should be surgically repaired as soon as possible (within 24 hours).
Hip fractures should be surgically repaired as soon as possible (within 24 hours).
![]() Delayed treatment of hip fractures in the elderly leads to increased complications and mortality.
Delayed treatment of hip fractures in the elderly leads to increased complications and mortality.
![]() General Considerations
General Considerations
Approximately 4% of the 7.9 million fractures that occur each year in the United States are hip fractures. There is a high mortality rate among elderly patients following hip fracture, with death occurring in 8–9% within 30 days and in approximately 25–30% within 1 year. Osteoporosis, female sex, height > 5-ft 8-in, and age over 50 years are risk factors for hip fracture. Hip fractures usually occur after a fall. High velocity trauma is needed in younger patients. Stress fractures can occur in athletes or individuals with poor bone mineral density following repetitive loading activities.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
Patients typically report pain in the groin, though pain radiating to the lateral hip, buttock, or knee can also commonly occur. If a displaced fracture is present, the patient will not be able to bear weight and the leg may be externally rotated. Gentle logrolling of the leg with the patient supine helps rule out a fracture. Examination of the hip demonstrates pain with deep palpation in the area of the femoral triangle (similar to palpating the femoral artery). Provided the patient can tolerate it, the clinician can, with the patient supine, flex the hip to 90 degrees with the knee flexed to 90 degrees. The leg can then be internally and externally rotated to assess the range of motion on both sides. Pain with internal rotation of the hip is the most sensitive test to identify intra-articular hip pathology. Hip flexion, extension, abduction, and adduction strength can be tested.
Patients with hip stress fractures have less pain on physical examination than described previously but typically have pain with weight bearing. The Trendelenburg test can be performed to examine for weakness or instability of the hip abductors, primarily the gluteus medius muscle (Table 10–5). Another functional test is asking the patient to hop or jump during the examination. If the patient has a compatible clinical history of pain and is unable or unwilling to hop, then a stress fracture should be ruled out. The back should be carefully examined in patients with hip complaints, including examining for signs for sciatica.
Table 10–5. Hip examination.

Following displaced hip fractures, a thorough medical evaluation and treatment should be pursued to maximize the patients’ ability to undergo operative intervention. Patients who are unable to get up by themselves may have been immobile for hours or even days following their falls. Thus, clinicians must exclude rhabdomyolysis, hypothermia, deep venous thrombosis, pulmonary embolism, and other conditions that can occur with prolonged immobilization. Delay of operative intervention leads to an increased risk of perioperative morbidity and mortality.
B. Imaging
Useful radiographic views of the hip include anteroposterior views of the pelvis and bilateral hips and frog-leg-lateral views of the painful hip. A CT scan or MRI may be necessary to identify the hip fracture pattern or to evaluate non-displaced fractures. Hip fractures are generally described by location, including femoral neck, intertrochanteric, or subtrochanteric.
![]() Treatment
Treatment
Almost all patients with a hip fracture will require surgery and may need to be admitted to hospital for pain control while they await surgery. Surgery is recommended within the first 24 hours because studies have shown that delaying surgery 48 hours results in at least twice the rate of major and minor medical complications, including pneumonia, decubitus ulcers, and deep venous thrombosis.
Stress fractures in active patients require a period of protected weight-bearing and a gradual return to activities, although it may take 4–6 months before a return to normal activities. Femoral neck fractures are commonly treated with hemiarthroplasty or total hip replacement. This allows the patient to begin weight-bearing immediately postoperatively. Peritrochanteric hip fractures are treated with open reduction internal fixation, where plate and screw construct or intramedullary devices are used. The choice of implant will depend on the fracture pattern. Since fracture fixation requires the fracture to proceed to union, the patient may need to have protected weight-bearing during the early postoperative period. Dislocation, periprosthetic fracture, and avascular necrosis of the hip are common complications after surgery.
Patients should be mobilized as soon as possible postoperatively to avoid pulmonary complications and decubitus ulcers. Supervised physical therapy and rehabilitation is important for the patient to regain as much function as possible. Unfortunately, most patients following hip fractures will lose some degree of independence.
![]() Prevention
Prevention
Bone density screening can identify patients at risk for osteopenia or osteoporosis, and treatment can be planned accordingly. Nutrition (calcium and vitamin D intake) and bone health (bone densitometry, serum calcium and 25-OH vitamin D levels) should be reviewed with the patient. For patients with decreased mobility, systemic anticoagulation with low-molecular-weight heparin or warfarin should be considered to avoid deep venous thrombosis. Fall prevention exercise programs are available for elderly patients at risk for falls and hip fractures. Hip protectors are uncomfortable and have less use in preventing fractures.
![]() When to Refer
When to Refer
All patients in whom hip fracture is suspected.
2. Osteoarthritis
ESSENTIALS OF DIAGNOSIS
![]() Pain deep in the groin on the affected side.
Pain deep in the groin on the affected side.
![]() Swelling.
Swelling.
![]() Degeneration of joint cartilage.
Degeneration of joint cartilage.
![]() Loss of active and passive range of motion in severe osteoarthritis.
Loss of active and passive range of motion in severe osteoarthritis.
![]() General Considerations
General Considerations
In the United States, the prevalence of osteoarthritis will grow as the number of persons over age 65 years doubles to more than 70 million by 2030. Cartilage loss and osteoarthritis symptoms are preceded by damage to the collagen-proteoglycan matrix. The etiology of osteoarthritis is often multifactorial, including previous trauma, prior high-impact activities, genetic factors, obesity, and rheumatologic or metabolic conditions.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
Osteoarthritis usually causes pain in the affected joint with loading of the joint or at the extremes of motion. Mechanical symptoms—such as swelling, grinding, catching, and locking—suggest internal derangement, which is indicated by damaged cartilage or bone fragments that affect the smooth range of motion expected at an articular joint. Pain can also produce the sensation of “buckling” or “giving way” due to muscle inhibition. As the joint degeneration becomes more advanced, the patient loses active range of motion and may lose passive range of motion as well.
Patients complain of pain deep in the groin on the affected side and have problems with weight-bearing activities such as walking, climbing stairs, and getting up from a chair. They may limp and develop a lurch during their gait, leaning toward the affected side as the walk to reduce pressure on the hip.
B. Imaging
Weight-bearing radiographs of the affected hip are preferred for evaluation of hip osteoarthritis. To reduce radiation exposure, obtain an anteroposterior weight-bearing radiograph of the pelvis with a lateral view of the symptomatic hip. Joint space narrowing and sclerosis suggest early osteoarthritis, while osteophytes near the femoral head or acetabulum and subchondral bone cysts are more advanced changes. After age 35, MRI of the hips already show labral changes in almost 70% of asymptomatic patients.
![]() Treatment
Treatment
A. Conservative
Changes in the articular cartilage are irreversible. Therefore, a cure for the diseased joint is not possible, although symptoms or structural issues can be addressed to try to maintain activity level. Conservative treatment for patients with osteoarthritis includes activity modification, therapeutic exercises, weight loss, and use of assistive devices (such as a cane). Lifestyle modifications also include proper footwear and avoidance of high impact activities.
Analgesics may be effective in some cases. Corticosteroid injections can be considered for short-term relief of pain; however, hip injections are best performed under fluoroscopic, ultrasound, or CT guidance to ensure accurate injection in the joint. Use of viscosupplementation in the hip has been studied with modest improvements; however, it remains an off-label use at this time.
B. Surgical
Two randomized trials demonstrate that arthroscopy does not improve outcomes at 1 year over placebo or routine conservative treatment of osteoarthritis. Arthroscopic surgery is indicated in patients with osteoarthritis if, rather than pain, they have mechanical symptoms and internal derangement symptoms that can be removed as the main complaint. Such surgical treatments are useful to restore range of motion by removing osteophytes, cartilage fragments, or loose bodies.
Joint replacement surgeries are effective and cost-effective for patients with significant symptoms and functional limitations, providing improvements in pain, function, and quality of life. Minimally invasive surgeries and computer-assisted navigation during operation are being investigated as methods to improve techniques (eg, accurate placement of the hardware implant) and to reduce complication rates.
Hip resurfacing surgery is a newer joint replacement technique. Rather than use a traditional artificial joint implant of the whole neck and femur, only the femoral head is removed and replaced. Concerns following resurfacing surgery include the risk of femoral neck fracture and collapse of the head. The cumulative survival rate of this implant at 10 years from recent studies is estimated to be 94%. Evidence so far suggests that hip resurfacing is comparable to total hip replacement and is a viable alternative for younger patients.
![]() When to Refer
When to Refer
Patients with sufficient disability, limited benefit from conservative therapy, and evidence of severe osteoarthritis can be referred for joint replacement surgery.
KNEE
1. Knee Pain
ESSENTIALS OF DIAGNOSIS
![]() Effusion can occur with intra-articular pathology, such as osteoarthritis, and meniscus and cruciate ligament tears.
Effusion can occur with intra-articular pathology, such as osteoarthritis, and meniscus and cruciate ligament tears.
![]() Acute knee swelling (hemarthrosis) within 2 hours may indicate ligament injuries or patellar dislocation or fracture.
Acute knee swelling (hemarthrosis) within 2 hours may indicate ligament injuries or patellar dislocation or fracture.
![]() General Considerations
General Considerations
The knee is the largest joint in the body and is susceptible to injury from trauma, inflammation, infection, and degenerative changes. The knee is a hinge joint. The joint line exists between the femoral condyles and tibial plateaus. Separating and cushioning these bony surfaces is the lateral and medial meniscal cartilage, which functions as a shock absorber during weight bearing, protecting the articular cartilage. The patella is a large sesamoid bone anterior to the joint. It is embedded in the quadriceps tendon, and it articulates with the trochlear groove of the femur. Poor patellar tracking in the trochlear groove is a common source of knee pain especially when the cause is atraumatic in nature. The knee is stabilized by the collateral ligaments against varus (lateral collateral ligament) and valgus (medial collateral ligament) stresses. The tibia is limited in its anterior movement by the anterior cruciate ligament (ACL) and in its posterior movement by the posterior cruciate ligament (PCL). The bursae of the knee are located between the skin and bony prominences. They are sac-like structures with a synovial lining. They act to decrease friction of tendons and muscles as they move over adjacent bony structures. Excessive external pressure or friction can lead to swelling and pain of the bursae. The prepatellar bursae (located between the skin and patella), and the pes anserine bursa (which is medial and inferior to the patella, just below the tibial plateau) are most commonly affected. Joint fluid, when excessive due to synovitis or trauma, can track posteriorly through a potential space, resulting in a popliteal cyst (also called a Baker cyst). Other structures that are susceptible to overuse injury and may cause knee pain following repetitive activity include the patellofemoral joint and the iliotibial band. Osteoarthritis of the knees is common after 50 years of age and can develop due to previous trauma, aging, activities, alignment issues, and genetic predisposition.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
Evaluation of knee pain should begin with general questions regarding duration and rapidity of symptom onset and the mechanism of injury or aggravating symptoms. Overuse or degenerative problems can occur with stress or compression from sports, hobbies, or occupation. A history of trauma, previous orthopedic problems with, or surgery to, the affected knee should also be specifically queried. Symptoms of infection (fever, recent bacterial infections, risk factors for sexually transmitted infections [such as gonorrhea] or other bacterial infections [such as staphylococcal infection]) should always be elicited.
Common symptom complaints include the following:
1. Presence of grinding, clicking, or popping with bending, may be indicative of osteoarthritis or the patellofemoral syndrome.
2. “Locking” or “catching” when walking suggests an internal derangement, such as meniscal injury or a loose body in the knee.
3. Intra-articular swelling of the knee or an effusion indicates an internal derangement or a synovial pathology. Large swelling may cause a popliteal (Baker) cyst. Acute swelling within minutes to hours suggests a hemarthrosis, most likely due to an ACL injury, fracture or patellar dislocation, especially if trauma is involved.
4. Lateral “snapping” with flexion and extension of the knee may indicate inflammation of the iliotibial band.
5. Pain that is worsened with bending and walking downstairs suggests issues with the patellofemoral joint, usually degenerative such as chondromalacia of the patella or osteoarthritis.
6. Pain that occurs when rising after prolonged sitting suggests a problem with tracking of the patella.
A careful history, coupled with a physical examination that includes observation, palpation and range of motion testing, as well as specific tests for particular anatomic structures is frequently sufficient to establish a diagnosis. When there is a knee joint effusion caused by increased fluid in the intra-articular space, physical examination will demonstrate swelling in the hollow or dimple around the patella and distention of the suprapatellar space.
Table 10–6 shows the differential diagnosis of knee pain, and Table 10–7 outlines possible diagnoses based on the location of pain.
Table 10–6. Differential diagnosis of knee pain.
Mechanical dysfunction or disruption
Internal derangement of the knee: injury to the menisci or ligaments
Degenerative changes caused by osteoarthritis
Dynamic dysfunction or misalignment of the patella
Fracture as a result of trauma
Intra-articular inflammation or increased pressure
Internal derangement of the knee: injury to the menisci or ligaments
Inflammation or infection of the knee joint
Ruptured popliteal (Baker) cyst
Peri-articular inflammation
Internal derangement of the knee: injury to the menisci or ligaments
Prepatellar or anserine bursitis
Ligamentous sprain
Table 10–7. Location of common causes of knee pain.
Medial knee pain
Medial compartment osteoarthritis
Medial collateral ligament strain
Medial meniscal injury
Anserine bursitis (pain over the proximal medial tibial plateau)
Anterior knee pain
Patellofemoral syndrome (often bilateral)
Osteoarthritis
Prepatellar bursitis (associated with swelling anterior to the patella)
“Jumper’s knee” (pain at the inferior pole of the patella)
Septic arthritis
Gout or other inflammatory disorder
Lateral knee pain
Lateral meniscal injury
Iliotibial band syndrome (pain superficially along the distal iliotibial band near lateral femoral condyle or lateral tibial insertion)
Lateral collateral ligament sprain (rare)
Posterior knee pain
Popliteal (Baker) cyst
Osteoarthritis
Meniscal tears
Hamstring or calf tendinopathy
B. Laboratory Findings
Laboratory testing of aspirated joint fluid, when indicated, can lead to a definitive diagnosis in most patients.
C. Imaging
Knee pain is evaluated with plain (weight-bearing) radiographs and MRI most commonly, but CT and ultrasound are sometimes useful.
An acute hemarthrosis represents bloody swelling that usually occurs within the first 1–2 hours following trauma. In situations where the trauma may be activity-related and not a result of a fall or collision, the differential diagnosis most commonly includes ACL tear (responsible for almost 50% of hemarthrosis in children and > 70% in adults), fracture (patella, tibial plateau, femoral supracondylar, growth plate [physeal]), and patellar dislocation. Meniscal tears are unlikely to cause large hemarthrosis.
2. Anterior Cruciate Ligament Injury
ESSENTIALS OF DIAGNOSIS
![]() An injury involving an audible pop when the knee buckles.
An injury involving an audible pop when the knee buckles.
![]() Acute swelling immediately (or within 4 hours).
Acute swelling immediately (or within 4 hours).
![]() Instability occurs with lateral movement activities and going down stairs.
Instability occurs with lateral movement activities and going down stairs.
![]() General Considerations
General Considerations
The anterior cruciate ligament (ACL) connects the posterior aspect of the lateral femoral condyle to the anterior aspect of the tibia. Its main function is to control anterior translation of the tibia on the femur. It also provides rotationally stability of the tibia on the femur. ACL tears are common with sporting injuries. They can result from both contact (valgus blow to the knee) and noncontact (jumping, pivoting, and deceleration) activities. The patient usually falls down following the injury, has acute swelling and difficulty with weight-bearing, and complains of instability. ACL injuries are common in skiing, soccer, football, and basketball among young adolescents and middle-age patients. Prepubertal and older patients usually sustain fractures instead of ligamentous injuries.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
Acute ACL injuries usually lead to acute swelling of the knee, causing difficulty with motion. After the swelling has resolved, the patient can walk with a “stiff-knee” gait or quadriceps avoidance gait because of the instability. More importantly, patients describe symptoms of instability while performing side-to-side maneuvers or descending stairs. Stability tests assess the amount of laxity of the knee while performing side-to-side maneuvers or descending stairs. The Lachman test (84–87% sensitivity and 93% specificity) is performed with the patient lying supine and the knee flexed to 20–30 degrees (Table 10–8). The clinician grasps the distal femur from the lateral side and the proximal tibia with the other hand on the medial side. With the knee in neutral position, stabilize the femur, and pull the tibia anteriorly using a similar force to lifting a 10- to 15-lb weight. Excessive anterior translation of the tibia compared with the other side indicates injury to the ACL. The anterior drawer test (48% sensitivity and 87% specificity) is performed with the patient lying supine and the knee flexed to 90 degrees (Table 10–8). The clinician stabilizes the patient’s foot by sitting on it and grasps the proximal tibia with both hands around the calf and pulls anteriorly. A positive test finds ACL laxity compared with the unaffected side. The pivot shift test is used to determine the amount of rotational laxity of the knee (Table 10–8). The patient is examined while lying supine with the knee in full extension. It is then slowly flexed while applying internal rotation and a valgus stress. The clinician feels for a subluxation at 20–40 degrees of knee flexion. The patient must remain very relaxed to have a positive test.
Table 10–8. Knee examination.




B. Imaging
Plain radiographs are usually negative in ACL tears but are useful to rule out fractures. A small avulsion injury can sometimes be seen over the lateral compartment of the knee. This is called a “Segond” fracture and is pathognomonic of an ACL injury. MRI is the best method to diagnose ACL tears. It has > 95% sensitivity and specificity for ACL tears. MRI also allows evaluation of other associated structures, such as menisci and cartilages.
![]() Treatment
Treatment
Most young and active patients will require surgical reconstruction of the ACL. Common surgical techniques use the patient’s own tissues, usually the patellar or hamstring tendons (autograft) or a cadaver graft (allograft) to arthroscopically reconstruct the torn ACL. Different patients groups experienced improved results with specific surgical graft choices. Recovery from surgery usually requires 6 months.
Nonoperative treatments are usually reserved for older patients or those with a very sedentary lifestyle. Physical therapy can focus on hamstring strengthening and core stability. An ACL brace can help stability. Longitudinal studies have demonstrated that nonoperative management of an ACL tear can lead to a higher incidence of meniscus tears. However, a small, randomized study demonstrated that acute ACL injuries may be treated nonoperatively initially, with similar clinical outcomes as those injuries that were operated on within 10 weeks of injury.
![]() When to Refer
When to Refer
• Almost all ACL tears should be referred to an orthopedic surgeon for evaluation.
• Individuals with instability in the setting of a chronic ACL tear (> 6 months) should be considered for surgical reconstruction.
• Patients with an ACL tear and associated meniscus or articular injuries may benefit from surgery to address the other injuries.
3. Collateral Ligament Injury
ESSENTIALS OF DIAGNOSIS
![]() Caused by a valgus or varus blow or stress to the knee.
Caused by a valgus or varus blow or stress to the knee.
![]() Pain and instability in the affected area.
Pain and instability in the affected area.
![]() Limited range of motion.
Limited range of motion.
![]() General Considerations
General Considerations
The medial collateral ligament (MCL) is the most commonly injured ligament in the knee. It is usually injured with a valgus stress to the partially flexed knee. It can also occur with a blow to the lateral leg. The MCL is commonly injured with acute ACL injuries. The lateral collateral ligament (LCL) is less commonly injured, but this can occur with a medial blow to the knee. Since both collateral ligaments are extra-articular, injuries to these ligaments may not lead to any intra-articular effusion. Affected patients may have difficulty walking initially, but this can improve when the swelling decreases.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
The main clinical findings for patients with collateral ligament injuries are pain along the course of the ligaments. The patient may have limited range of motion due to pain, especially during the first 2 weeks following the injury. The best tests to assess the collateral ligaments are the varus and valgus stress tests. The sensitivity of the tests is as high as 86–96%.
The valgus stress test is performed with the patient supine (Table 10–8). The clinician should stand on the outside of the patient’s knee. With one hand, the clinician should hold the ankle while the other hand is supporting the leg at the level of the knee joint. A valgus stress is applied at the ankle to determine pain and laxity of the MCL. The test should be performed at both 30 degrees and 0 degrees of knee extension.
For the varus stress test, the patient is again placed supine (Table 10–8). For the right knee, the clinician should be standing on the right side of the patient. The clinician’s left hand should be holding the ankle while the right hand is supporting the lateral thigh. A varus stress is applied at the ankle to determine pain and laxity of the LCL. The test should be performed at both 30 degrees and 0 degrees of knee flexion.
The test results can be graded from 1–3. Grade 1 is when the patient has pain with varus/valgus stress test but no instability. With grade 2 injuries, the patient has pain, and the knee shows instability at 30 degrees of knee flexion. In grade 3 injuries, the patient has marked instability but not much pain. The knee is often unstable at both 30 degrees and 0 degrees of knee flexion.
B. Imaging
Radiographs are usually nondiagnostic except for avulsion injuries. However, radiographs should be used to rule out fractures that can occur with collateral ligament injuries. Isolated MCL injuries usually do not require evaluation by MRI, but MRI should be used to evaluate possible associated cruciate ligament injuries. LCL or posterolateral corner injuries should have MRI evaluation to exclude associated injuries and to determine their significance.
![]() Treatment
Treatment
The majority of MCL injuries can be treated with protected weight-bearing and physical therapy. For grade 1 and 2 injuries, the patient can usually bear weight as tolerated with full range of motion. A hinged knee brace can be given to patients with grade 2 MCL tears to provide stability. Early physical therapy is recommended to protect range of motion and muscle strength. Grade 3 MCL injuries require long leg braces to provide stability. Patients can weight-bear but only with the knee locked in extension with a brace. The motion can then be increased with the brace unlocked. Grade 3 injuries can take up to 6–8 weeks to heal. MCL injuries rarely need surgery. LCL injuries usually require surgical repair or reconstruction.
![]() When to Refer
When to Refer
• Symptomatic instability with chronic MCL tears or acute MCL tears with other ligamentous injuries.
• LCL or posterolateral corner injuries require urgent surgical repair or reconstruction (within 1 week).
4. Posterior Cruciate Ligament Injury
ESSENTIALS OF DIAGNOSIS
![]() Usually follows an anterior trauma to the tibia, such as a dashboard injury during a motor vehicle accident.
Usually follows an anterior trauma to the tibia, such as a dashboard injury during a motor vehicle accident.
![]() The knee may freely dislocate and reduce.
The knee may freely dislocate and reduce.
![]() One-third of multi-ligament injuries involving the PCL have neurovascular injuries.
One-third of multi-ligament injuries involving the PCL have neurovascular injuries.
![]() General Considerations
General Considerations
The posterior cruciate ligament (PCL) is the strongest ligament in the knee. PCL injuries usually represent significant trauma and are highly associated with multi-ligament injuries and knee dislocations. More than 70–90% of PCL injuries have associated injuries to the posterolateral corner, MCL, and ACL. There should be high suspicion for neurovascular injuries and a thorough neurovascular examination of the limb should be performed.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
Most patients with acute injuries have difficulty with ambulation. Patients with chronic PCL injuries can ambulate without gross instability but may complain of subjective “looseness” and often report pain and dysfunction, especially with bending. Clinical examinations of PCL injuries include the “sag sign” (Table 10–8). The patient is placed supine and both hips and knees are flexed up to 90 degrees. Because of gravity, the PCL-injured knee will have an obvious set-off at the anterior tibia that is “sagging” posteriorly. The PCL ligament can also be examined using the posterior drawer test (90% sensitivity and 99% specificity) (Table 10–8). The patient is placed supine with the knee flexed at 90 degrees. In a normal knee, the anterior tibia should be positioned about 10 mm anterior to the femoral condyle. The clinician can grasp the proximal tibia with both hands and push the tibia posteriorly. The movement, indicating laxity and possible tear of the PCL, is compared with the uninjured knee. A PCL injury is sometimes mistaken for an ACL injury during the anterior drawer test since the tibia is subluxed posteriorly in a sagged position and can be abnormally translated forward, yielding a false-positive test for an ACL injury. Pain, swelling, pallor, and numbness in the affected extremity may suggest a knee dislocation with possible injury to the popliteal artery.
B. Imaging
Radiographs are often nondiagnostic but are required to diagnose any fractures. MRI is used to diagnose PCL and other associated injuries.
![]() Treatment
Treatment
Isolated PCL injuries can be treated nonoperatively. Acute injuries are usually immobilized using a knee brace with the knee extension; the patient uses crutches for ambulation. Physical therapy can help achieve increased range of motion and improved ambulation. Many PCL injuries are associated with other injuries and may require operative reconstruction. Neurovascular injuries occur in up to one-third of all knee dislocations or PCL injuries.
![]() When to Refer
When to Refer
• The patient should be seen urgently within 1–2 weeks.
• If the lateral knee is also unstable with varus stress testing, the patient should be assessed for a posterolateral corner injury, which may require an urgent surgical reconstruction.
• Isolated PCL tears may require surgery if the tear is complete (grade 3) and the patient is symptomatic.
5. Meniscus Injuries
ESSENTIALS OF DIAGNOSIS
![]() Patient may or may not report an injury.
Patient may or may not report an injury.
![]() Joint line pain and pain with deep squatting are the most sensitive signs.
Joint line pain and pain with deep squatting are the most sensitive signs.
![]() Difficulty with knee extension suggests an internal derangement that should be evaluated urgently with MRI.
Difficulty with knee extension suggests an internal derangement that should be evaluated urgently with MRI.
![]() General Considerations
General Considerations
The menisci act as shock absorbers within the knee. Injuries to a meniscus can lead to pain, clicking, and locking sensation. Most meniscus injuries occur with acute injuries (usually in younger patients) or repeated microtrauma, such as squatting or twisting (usually in older patients).
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
The patient may have an antalgic (painful) gait and difficulty with squatting. He or she may complain of catching or locking of the meniscal fragment. Physical findings can include effusion or joint line tenderness. Patients can usually point out the area of maximal tenderness along the joint line. Swelling usually occurs during the first 24 hours after the injury or later. Meniscus tears rarely lead to the immediate swelling that is commonly seen with fractures and ligament tears. Meniscus tears are commonly seen in arthritic knees. However, it is often unclear whether the pain is coming from the meniscus tear or the arthritis.
Provocative tests, including the McMurray test, the modified McMurray test, and the Thessaly test, can be performed to confirm the diagnosis (Table 10–8). Most symptomatic meniscus tears cause pain with deep squatting and when waddling (performing a “duck walk”).
B. Imaging
Radiographs are usually normal but may show joint space narrowing, early osteoarthritis changes, or loose bodies. MRI of the knee is the best diagnostic tool for meniscal injuries (93% sensitivity and 95% specificity). High signal through the meniscus (bright on T2 images) represents a meniscal tear.
![]() Treatment
Treatment
Conservative treatment can be used for degenerative tears in older patients. The treatment is similar for patients with mild knee osteoarthritis, including analgesics and physical therapy for strengthening and core stability. Acute tears in young and active patients can be best treated arthroscopically with meniscus repair or debridement. Randomized controlled studies have demonstrated no benefit with arthroscopic meniscectomy in patients with advanced osteoarthritis.
![]() When to Refer
When to Refer
• If the patient has symptoms of internal derangement suspected as meniscus injury. The patient should receive an MRI to confirm the injury.
• If the patient cannot extend the knee due to a mechanical block, the patient should be evaluated as soon as possible. Certain shaped tears on MRI, such as bucket handle tears, are amenable to meniscal repair surgery.
6. Patellofemoral Pain
ESSENTIALS OF DIAGNOSIS
![]() Pain experienced with bending activities (kneeling, squatting, climbing stairs).
Pain experienced with bending activities (kneeling, squatting, climbing stairs).
![]() Lateral deviation or tilting of the patella in relation to the femoral groove.
Lateral deviation or tilting of the patella in relation to the femoral groove.
![]() General Considerations
General Considerations
Patellofemoral pain, also known as anterior knee pain or “runner’s knee,” describes any pain involving the patellofemoral joint. The pain affects any or all of the anterior knee structures, including the medial and lateral aspects of the patella as well as the quadriceps and patellar tendon insertions. The patella engages the femoral trochlear groove with approximately 30 degrees of knee flexion. Forces on the patellofemoral joint increase up to three times body weight as the knee flexes to 90 degrees (eg, climbing stairs), and five times body weight when going into full knee flexion (eg, squatting). Abnormal patellar tracking during flexion can lead to abnormal articular cartilage wear and pain. When the patient has ligamentous hyperlaxity, the patella can sublux out of the groove, usually laterally. Patellofemoral pain is also associated with muscle strength and flexibility imbalances as well as altered hip and ankle biomechanics.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
Patients usually complain of pain in the anterior knee with bending movements and less commonly in full extension. Pain from this condition is localized under the kneecap but can sometimes be referred to the posterior knee or over the medial or lateral inferior patella. Symptoms may begin after a trauma or after repetitive physical activity, such as running and jumping. When maltracking, palpable and sometimes audible crepitus can occur.
Intra-articular swelling usually does not occur unless there are articular cartilage defects or if osteoarthritis changes develop. On physical examination, it is important to palpate the articular surfaces of the patella. For example, the clinician can use one hand to move the patella laterally, and use the fingertips of the other hand to palpate the lateral undersurface of patella. Patellar mobility can be assessed by medially and laterally deviating the patella (deviation by one-quarter of the diameter of the kneecap is consider normal; greater than one-half the diameter suggests excessive mobility). The apprehension signsuggests instability of the patellofemoral joint and is positive when the patient becomes apprehensive when the patella is deviated laterally (Table 10–8). The patellar grind test is performed by grasping the knee superior to the patella and pushing it downward with the patient supine and the knee extended, pushing the patella inferiorly. The patient is asked to contract the quadriceps muscle to oppose this downward translation, with reproduction of pain or grinding being the positive sign for chondromalacia of the patella. There are two common presentations: (1) Patients whose ligaments and patella are too loose (hypermobility); (2) and patients who have soft tissues that are too tight leading to excessive pressure on the joint.
Evaluation of the quadriceps strength and hip stabilizers can be accomplished by having the patient perform a one-leg squat without support. Patients who are weak may display poor balance, with dropping of the pelvis (similar to a positive hip Trendelenburg sign) or excessive internal rotation of the knee medially. Normally, with a one-leg squat, the knee should align over the second metatarsal ray of the foot.
B. Imaging
Diagnostic imaging has limited use in younger patients and is more helpful in older patients to assess for osteoarthritis or to evaluate patients who do not respond to conservative treatment. Radiographs may show lateral deviation or tilting of the patella in relation to the femoral groove. MRI may show thinning of the articular cartilage but is not clinically necessary, except prior to surgery or to exclude other pathology.
![]() Treatment
Treatment
A. Conservative
For symptomatic relief, use of local modalities such as ice and anti-inflammatory medications can be beneficial. If the patient has signs of patellar hypermobility, physical therapy exercises are useful to strengthen the quadriceps (especially the vastus medialis obliquus muscle) to help stabilize the patella and improve tracking. Support for the patellofemoral joint can be provided by use of a patellar stabilizer brace or special taping techniques (McConnell taping). Correcting lower extremity alignment (with appropriate footwear or over-the-counter orthotics) can help improve symptoms, especially if the patient has pronation or high arched feet. If the patient demonstrates tight peripatellar soft tissues, special focus should be put on stretching the hamstrings, iliotibial band, quadriceps, calves, and hip flexors. Strengthening exercises should include the quadriceps and hip abductors.
B. Surgical
Surgery is rarely needed and is considered a last resort for patellofemoral pain. Procedures performed include lateral release or patellar realignment surgery.
When to Refer
Patients with persistent symptoms.
7. Osteoarthritis
ESSENTIALS OF DIAGNOSIS
![]() Degeneration of joint cartilage.
Degeneration of joint cartilage.
![]() Pain with bending or twisting activities.
Pain with bending or twisting activities.
![]() Swelling.
Swelling.
![]() Loss of active and passive range of motion in severe osteoarthritis.
Loss of active and passive range of motion in severe osteoarthritis.
![]() General Considerations
General Considerations
In the United States, the prevalence of osteoarthritis will grow as the number of persons over age 65 years doubles to more than 70 million by 2030. The incidence of knee osteoarthritis in the United States is 240 per 100,000 person-years.
Cartilage loss and osteoarthritis symptoms are preceded by damage to the collagen-proteoglycan matrix. The etiology of osteoarthritis is often multifactorial including previous trauma, prior high-impact activities, genetic factors, obesity, and rheumatologic or metabolic conditions.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
Osteoarthritis usually causes pain in the affected joint with loading of the joint or at the extremes of motion. Mechanical symptoms—such as swelling, grinding, catching, and locking—suggest internal derangement, which is indicated by damaged cartilage or bone fragments that affect the smooth range of motion expected at an articular joint. Pain can also produce the sensation of “buckling” or “giving way” due to muscle inhibition. As the joint degeneration becomes more advanced, the patient loses active range of motion and may lose passive range of motion as well.
As the condition worsens, patients with knee osteoarthritis have an increasingly limited ability to walk. Symptoms include pain with bending or twisting activities, and going up and down stairs. Swelling, limping, and pain while sleeping are common complaints with osteoarthritis, especially as it progresses.
B. Imaging
The most commonly recommended radiographs include bilateral weight-bearing 45-degree bent knee posteroanterior, lateral, and patellofemoral joint views (Merchant view). Radiographic findings include diminished width of the articular cartilage causing joint space narrowing, subchondral sclerosis, presence of osteophytes, and cystic changes in the subchondral bone. MRI of the knee is most likely unnecessary unless other pathology is suspected, including ischemic osteonecrosis of the knee.
![]() Treatment
Treatment
A. Conservative
Changes in the articular cartilage are irreversible. Therefore, a cure for the diseased joint is not possible, although symptoms or structural issues can be addressed to try to maintain activity level. Conservative treatment for all patients with osteoarthritis includes activity modification, therapeutic exercises, and weight loss. Lifestyle modifications also include proper footwear and avoidance of high impact activities.
Use of a cane in the hand opposite to the affected side is mechanically advantageous. Knee sleeves or braces provide some improvement in subjective pain symptoms most likely due to improvements in neuromuscular function. If patients have unicompartmental osteoarthritis in the medial or lateral compartment, joint unloader braces are available to offload the degenerative compartment. Cushioning footwear and appropriate orthotics or shoe adjustments are useful for reducing impact to the lower extremities.
The initial drugs of choice for the treatment of pain in knee osteoarthritis are oral acetaminophen and topical capsaicin. If a traditional NSAID is indicated, the choice should be based on cost, side-effect profile, and adherence. The cyclooxygenase (COX)-2 inhibitor, celecoxib, is no more effective than traditional NSAIDs; it may offer short-term, but probably not long-term, advantage in preventing gastrointestinal complications. Due to its cost and potential cardiovascular risk, celecoxib should be reserved for carefully selected patients. The role of topical NSAIDs are being considered in the osteoarthritis treatment algorithm, as they do avoid many of the traditional NSAID complications. Opioids can be used appropriately in patients with severe osteoarthritis. Glucosamine and chondroitin sulfate are supplements that have been widely used and marketed for osteoarthritis. Evidence for their effectiveness in slowing or reversing cartilage loss is limited and any effect present appears to be small. Despite some initial promise, the best-controlled studies indicate these supplements are ineffective as analgesics in osteoarthritis. However, they have minimal side effects and may be appropriate if the patient experiences subjective benefit.
Knee joint corticosteroid injections are options to help reduce pain and inflammation and can provide short-term pain relief, usually lasting about 6–12 weeks. Viscosupplementation by injections of hyaluronic acid-based products improves synovial fluid viscosity by increasing the molecular weight and quantity of hyaluronic acid beyond that naturally synthesized by the synovium. Laboratory studies also demonstrate that hyaluronic acid injections decrease inflammatory cytokines and free radicals. Studies also demonstrate more prolonged effects of viscosupplementation products compared with corticosteroid injection with symptom improvement for > 6 months in some patients with mild knee osteoarthritis. A recent meta-analysis questions the value of viscosupplementation suggesting only a small and clinically irrelevant benefit and an increased risk of serious adverse events. However, older meta-analyses found modest improvements and did not report similar concerns regarding serious side effects.
B. Surgical
Two randomized trials demonstrate that arthroscopy does not improve outcomes at 1 year over placebo or routine conservative treatment of osteoarthritis. Arthroscopic surgery is indicated in patients with osteoarthritis if, rather than pain, they have mechanical symptoms and internal derangement symptoms. Such surgical treatments are useful to restore range of motion by removing osteophytes, cartilage fragments, or loose bodies.
Joint replacement surgeries are effective and cost-effective for patients with significant symptoms or functional limitations, providing improvements in pain, function, and quality of life. The number of total knee arthroplasty procedures jumped 162% from 1991 to 2010, along with an increase in complications and hospital readmissions. Minimally invasive surgeries and computer-assisted navigation during operation are being investigated as methods to improve techniques (eg, accurate placement of the hardware implant) and to reduce complication rates.
Knee realignment surgery, such as high tibial osteotomy or partial knee replacement surgery, is indicated in patients younger than age 60 with unicompartmental osteoarthritis, who would benefit from delaying total knee replacement. Knee joint replacement surgery has been very successful in improving outcomes for patient with end-stage osteoarthritis. Recent long-term series describe > 95% survival rate of the implant at 15 years.
![]() When to Refer
When to Refer
Patients with sufficient disability, limited benefit from conservative therapy, and evidence of severe osteoarthritis can be referred for joint replacement surgery.
ANKLE INJURIES
1. Inversion Ankle Sprains
ESSENTIALS OF DIAGNOSIS
![]() Localized pain and swelling.
Localized pain and swelling.
![]() The majority of ankle injuries involve inversion injuries affecting the lateral ligaments.
The majority of ankle injuries involve inversion injuries affecting the lateral ligaments.
![]() Consider chronic ankle instability or associated injuries if pain persists for > 3 months following an ankle sprain.
Consider chronic ankle instability or associated injuries if pain persists for > 3 months following an ankle sprain.
![]() General Considerations
General Considerations
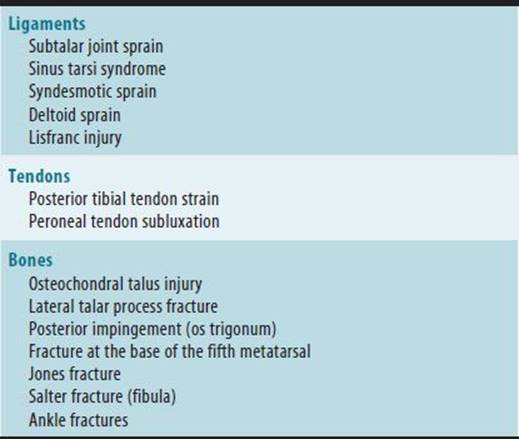
Ankle sprains are the most common sports injuries seen in outpatient clinics. Patients usually report “turning the ankle” during a fall or after landing on an irregular surface such as a hole or an opponent’s foot. The most common mechanism of injury is an inversion and plantarflexion sprain, which injures the anterior talofibular ligament (ATF) ligament rather than the calcaneofibular ligament (CF) ligament. Other injuries that can occur with inversion ankle injuries are listed in (Table 10–9).
Table 10–9. Injuries associated with ankle sprains.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
The usual symptoms following a sprain include localized pain and swelling over the lateral aspect of the ankle, difficulty weight bearing, and limping. The patient’s ankle may feel unstable. On examination, there may be swelling or bruising over the lateral aspect of the ankle. The anterior, inferior aspect below the lateral malleolus is most often the point of maximal tenderness consistent with ATF and CF ligament injuries. The swelling may limit motion of the ankle. Special stress tests for the ankle include the anterior drawer test (Table 10–10) and subtalar tilt test (Table 10–10). In order to grade the severity of ankle sprains, no laxity on stress tests is considered a grade 1 injury, laxity of the ATF ligament on anterior drawer testing but a negative tilt test is a grade 2 injury, and both positive drawer and tilt tests signify a grade 3 injury.
Table 10–10. Ankle examination.

B. Imaging
Routine ankle radiographic views include the anteroposterior, lateral, and oblique (mortise) views. Less common views requested include the calcaneal view and subtalar view. Ottawa Ankle Rules are clinical prediction rules to guide the need for radiographs and have a 97% sensitivity and 99% negative predictive value. If the patient is unable to bear weight immediately in the office setting or emergency department for four steps, then the clinician should check for (1) bony tenderness at the posterior edge of the medial or lateral malleolus and (2) bony tenderness over the navicular (medial midfoot) or at the base of the fifth metatarsal. If either malleoli demonstrates pain or deformity, then ankle radiographs should be obtained. If the foot has bony tenderness, obtain foot radiographs. An MRI is helpful when considering the associated injuries.
![]() Treatment
Treatment
Immediate treatment of an ankle sprain follows the MICE mnemonic: modified activities, ice, compression, and elevation. Subsequent treatment involves protected weight bearing with crutches and use of an ankle stabilizer brace, especially for grade 2 and 3 injuries. Early motion is essential, and patients should be encouraged to do home exercises or physical therapy. Proprioception and balance exercises (eg, “wobble board”) are useful to restore function to the ankle and prevent future ankle sprains. Regular use of an ankle support with activities can reduce the risk of lateral ankle sprains. Chronic instability can develop after acute ankle sprain in 10–20% of people and may require surgical stabilization with ligament reconstruction surgery.
![]() When to Refer
When to Refer
• Ankle fractures.
• Recurrent ankle sprains or signs of chronic ligamentous ankle instability.
• No response after more than 3 months of conservative treatment.
• Suspicion of associated injuries.
2. Eversion (“High”) Ankle Sprains
ESSENTIALS OF DIAGNOSIS
![]() Severe and prolonged pain.
Severe and prolonged pain.
![]() Limited range of motion.
Limited range of motion.
![]() Mild swelling.
Mild swelling.
![]() Difficulty with weight bearing.
Difficulty with weight bearing.
![]() General Considerations
General Considerations
A syndesmotic injury or “high ankle” sprain involves the anterior tibiofibular ligament in the anterolateral aspect of the ankle, superior to the anterior talofibular (ATF) ligament. The injury mechanism often involves the foot being turned out or externally rotated and everted (eg, when being tackled). This injury is commonly missed or misdiagnosed as an ATF ligament sprain on initial visit.
![]() Clinical Findings
Clinical Findings
A. Symptoms and Signs
Symptoms of a high ankle sprain include severe and prolonged pain over the anterior ankle at the anterior tibiofibular ligament, worse with weight bearing. This is often more painful than the typical ankle sprain. The point of maximal tenderness involves the anterior tibiofibular ligament, which is higher than the ATF ligament. It is also important to palpate the proximal fibula to rule out any proximal syndesmotic ligament injury and associated fracture known as a “maisonneuve fracture.” There is often some mild swelling in this area, and the patient may or may not have an ankle effusion. The patient usually has limited range of motion in all directions. The external rotation stress test reproduces the mechanism of injury (Table 10–10). (Note: The patient’s foot should have an intact neurovascular examination before undertaking this test.)
B. Imaging
Radiographs of the ankle should include the anteroposterior, mortise, and lateral views. The mortise view may demonstrate loss of the normal overlap between the tibia and fibula, which should be at least 1–2 mm. Asymmetry in the joint space around the tibiotalar joint suggests disruption of the syndesmotic ligaments. If there is proximal tenderness in the lower leg especially around the fibula, an anteroposterior and lateral view of the tibia and fibula should be obtained to rule out a proximal fibula fracture. Radiographs during an external rotation stress test may visualize instability at the distal tibiofibular joint. MRI is the best method to visualize injury to the tibiofibular ligament and to assess status of the other ligaments and the articular cartilage.
![]() Treatment
Treatment
Whereas most ankle sprains are treated with early motion and weight bearing, treatment for a high ankle sprain should be conservative with a cast or walking boot for 4–6 weeks. Thereafter, protected weight bearing with crutches is recommended until the patient can walk pain-free. Physical therapy can start early to regain range of motion and maintain strength with limited weight-bearing initially.
![]() When to Refer
When to Refer
If there is widening of the joint space and asymmetry at the tibiotalar joint, the patient should be referred urgently to a foot and ankle surgeon. Severe or prolonged persistent cases that do not heal may require internal fixation to avoid chronic instability at the tibiofibular joint.
REFERENCES
Al Nezari NH: Neurological examination of the peripheral nervous system to diagnose lumbar spinal disc herniation with suspected radiculopathy. Spine J 2013;13:657 [PMID: 23499340].
Ammendolia C: Nonoperative treatment of lumbar spinal stenosis with neurogenic claudication. Spine 2012;37:E609 [PMID: 22158059].
Iversen T: Accuracy of physical examination for chronic lumbar radiculopathy. BMC Musculoskelet Disord 2013;14:206 [PMID: 23837886].
Kelly JC: The natural history and clinical syndromes of degenerative cervical spondylosis. Adv Orthop 2012;2012:393642 [PMID: 22162812].
Kemler E: A systematic review on the treatment of acute ankle sprain. Sports Med 2011;41:185 [PMID: 21395362].
Radcliff K: Epidural steroid injections are associated with less improvement in patients with lumbar spinal stenosis. Spine 2013;38:279 [PMID: 23238485].
Rihn JA: Duration of symptoms resulting from lumbar disc herniation. J Bone Joint Surg Am 2011;93:1906 [PMID: 22012528].
Rubinstein SM: Spinal manipulative therapy for acute low back pain. Spine 2013;38:158 [PMID: 23169072].
Suri P: Recurrence of radicular pain or back pain after nonsurgical treatment of symptomatic lumbar disk herniation. Arch Phys Med Rehabil 2012;93:690 [PMID: 22464091].
Tijssen M: Diagnostics of femoroacetabular impingement and labral pathology of the hip. Arthroscopy 2012;28:860 [PMID: 22365268].
Visser LH: Sciatica-like symptoms and the sacroiliac joint: clinical features and differential diagnosis. Eur Spine J 2013;22:1657 [PMID: 23455949].
Willems P: Decision making in surgical treatment of chronic low back pain: the performance of prognostic tests to select patients for lumbar spinal fusion. Acta Orthop Suppl 2013;84:1 [PMID: 23427903].
![]() SELF-ASSESSMENT QUESTIONS
SELF-ASSESSMENT QUESTIONS
Select the one correct answer for each question.
Question 1: Low back pain
a. seldom resolves within 2 weeks
b. nearly always resolves within 6 weeks
c. is not a presenting symptom in other serious medical problems
d. is unrelated to degenerative changes in the lumbar spine
Question 2: Spinal stenosis
a. is a narrowing of the spinal canal unrelated to osteoarthritis
b. is typically the result of a disk herniation
c. causes pain that worsens with flexion
d. may present with neurogenic claudicaction symptoms with walking
Question 3: Lumbar disk herniation
a. is the most common occupational injury
b. must have a plausible history of an inciting incident
c. does not occur from degenerative disk disease
d. nearly always affects the L5–S1 disk
Question 4: Hip fractures
a. should be surgically repaired as soon as possible (within 24 hours)
b. can be entirely prevented with exercise programs
c. can be entirely prevented with hip protectors
d. should not be subjected to internal rotation of the hip
Question 5: Osteoarthritis
a. should never be treated with corticosteroids
b. can be reversed with anti-inflammatory drugs
c. involves a degeneration of the joint cartilage
d. is not affected by repetitive trauma
Question 6: Anterior cruciate ligament injury
a. impacts rotational stability of the tibia on the patella
b. is usually a painless buckling of the knee
c. causes instability going up more than down stairs
d. leads to acute swelling immediately (or within 4 hours)
Question 7: Collateral ligament injury
a. is caused by a valgus or varus blow or stress to the knee
b. is usually caused by a valgus stress to the partially extended knee
c. seldom presents with pain along the course of the ligaments
d. is assessed by the varus and valgus stress tests despite their lack of sensitivity
Question 8: Inversion ankle sprains
a. may result in chronic instability
b. never require surgical stabilization with ligament reconstruction
c. require MRI to rule out associated injuries
d. are treated in the same manner as eversion (high) ankle sprains
Chapter adapted, with permission, from Luke A, Ma CB. Sports medicine and outpatient orthopedics. In: Papadakis MA, McPhee SJ, Rabow MW, eds. Current Medical Diagnosis and Treatment. 53rd ed. New York: McGraw-Hill; 2014.