Richard E. Burney
Presentation
A 40-year-old woman comes to your office for an urgent visit complaining of severe anal pain and tenderness that has developed over the past 2 days. She has no history of prior rectal complaints or change in bowel habit. There is no history of abdominal pain, diarrhea, or blood in her stools. On examination, she appears healthy and is afebrile. Examination of the perianal area reveals an erythematous, tender area about 1.5 cm in diameter at the posterior anal verge. It appears fluctuant. Gentle palpation is exquisitely painful precluding further rectal examination.
Differential Diagnosis
In evaluating the patient with acute pain and swelling in the perianal and buttock region, one must keep in mind both the possible etiologies and the anatomy of the region, in particular the various locations or spaces where infection and abscess can arise and be manifest. There are many possible etiologies of perianal and perirectal infection, ranging from anal gland infection, to defecation-related anal canal trauma, to inflammatory bowel disease. The specific etiology, however, is not of immediate concern at the time of acute presentation when prompt diagnosis and surgical management of abscess take precedence.
The first step in the differential diagnosis of acute anal pain and swelling is to distinguish between perianal abscess, which is painful but unlikely to cause serious illness or sequelae, and perirectal or ischiorectal abscess, which can be highly morbid and life threatening if treatment is delayed or inadequate (Figure 1).

FIGURE 1 • Schematic drawing showing typical locations of perianal and perirectal abscess. Locations of abscesses can be variable and do not necessarily conform to these locations.
Perianal abscess is limited in extent and location to the perianal tissues and intersphincteric plane, the avascular space between the internal and the external sphincter muscles. Perianal abscesses are small and do not penetrate laterally through the anal sphincter into the ischiorectal fossa tissues or upward into the supralevator space. The swelling of a perianal abscess is usually readily visible and easily palpable at the anal verge and does not give rise to signs of systemic infection (Figure 2).

FIGURE 2 • Perianal abscess.
Closely related to perianal abscess, and possibly its precursor, is intersphincteric abscess. An intersphincteric abscess is also small, and so named because it develops in the avascular plane between the internal and the external sphincter. Unlike perianal abscess, which is usually visible under the perianal skin, it causes no outward visible signs. It causes pain and tenderness more so in the anal canal than on the surface. Tenderness is usually exquisite and elicited during rectal examination by palpation in the anal canal. The diagnosis of intersphincteric abscess can be difficult because the signs are subtle. Intersphincteric abscess if untreated may simply evolve into a perianal abscess, which is easier to diagnose, but it could also extend upward or outward leading to a much more serious supralevator or ischiorectal abscess.
Ischiorectal abscess develops when infection, which originates in the intersphincteric space, penetrates through the external sphincter and enters the larger, fatfilled space of the ischiorectal fossa where a much larger abscess can develop (Figure 3). Patients with ischiorectal abscess will usually have fever, elevated white blood cell count, and may have signs of sepsis. The medial buttock will be erythematous, swollen, and tender. Because the abscess may be quite deep, more than 2 to 3 cm under the skin, obvious fluctuance is not always present. On rectal examination, one may feel a ballotable mass between the buttock and the lower rectum, which is more obvious when done under anesthesia. Perirectal abscesses are easily seen on CT, but CT should not be needed to make this diagnosis in most patients.

FIGURE 3 • Appearance of ischiorectal abscess. Scar is from I&D of previous abscess.
High intersphincteric or supralevator abscesses are rare and are the most difficult to diagnose and treat. Patients will have had rectal pain, with or without fever, usually for several days or more. External examination is unrevealing. On careful rectal examination, one may be able to feel a fluctuant mass high in the anal canal at the level of the levator or anorectal ring, but physical findings can be quite subtle. WBC count may be elevated. CT imaging of the pelvis, which is being done with increasing regularity in situations such as this, where one has a patient with unexplained rectal pain and signs of infection, can be very helpful in identifying the presence and exact location of these occult abscesses.
Patients can also develop simple perianal carbuncles, or simple abscesses involving the perianal or buttock skin and superficial subcutaneous tissues, which have no etiologic relation to anal canal structures (Figure 4). Pilonidal abscess is usually located in the buttock cleft, well away from the anus. Sinus tracts arising from pilonidal cyst on occasion find their way to the perianal buttock tissues and when this happens can mimic ischiorectal abscess. Sebaceous cysts in the perianal skin can become infected and lead to abscess in the perianal region. When this happens, the patient may give a history of having had a lump there for some time that has suddenly become more tender and swollen. Finally, perianal hidradenitis suppurativa can cause anal pain and swelling. These patients rarely have disease limited to the perianal region, however, and almost always give a history of chronic pain, swelling, and drainage.

FIGURE 4 • Carbuncle on buttock (Staph aureus).
The differential diagnosis of patients with anal pain also includes such entities as acute hemorrhoidal inflammation, acute thrombosed hemorrhoid, acute anal fissure, anorectal inflammatory bowel disease flare, and neoplasm. None of these entities will cause fever or WBC count elevation. Patients with anorectal inflammatory bowel disease usually have other visible abnormalities and tissue distortion in the perianal area that is characteristic (Figure 5). Nevertheless, they may have local swelling and abscess, or ulceration that mimics abscess in its symptoms. Acute hemorrhoidal swelling and thrombosed hemorrhoids are visible and should be easily identified on external examination. By history, patients with anal fissure have anal bleeding and pain with defecation, followed by a burning or “razor blade” sensation that can last for up to an hour or more. Anal fissure can be identified most easily by simply stretching the perianal skin to expose the fissure in the anal canal. There is no swelling and tenderness is limited to the site of the fissure itself.

FIGURE 5 • Anal inflammation from Crohn’s disease showing inflammatory tags, edema, and ulceration.
Patients with fistula in ano will most often give a history of chronic perianal drainage or intermittent, recurrent swelling and drainage from a perianal location, usually within 3 to 4 cm of the anal verge. Acute pain and swelling may be intermittently felt, but are not prominent symptoms of anal fistula. A small nubbin of granulation tissue may be present at the external fistula opening. A small proportion of patients who have undergone drainage of perianal abscess may later be found to have an associated or underlying fistula in ano, but in my experience these fistulae are rarely evident at the time of surgical incision and drainage. There is no need to spend extra time looking for a possible fistula if it is not obvious at the time of initial surgical incision and drainage. If an underlying fistula is present, it will become apparent in time. Most patients with fistula in ano do not initially present with an abscess; most patients with abscess do not go on to develop fistula in ano.
Workup
The most important parts of the workup for anal pain and swelling are a complete history and a careful physical examination. The history should define the exact time course of symptoms and their specific nature. Temperature and pulse rate may give a clue as to depth and extent of abscess. Physical examination must include careful inspection and palpation of the buttock and perianal region, preferably with the patient in a knee-chest position on a sigmoidoscopy or similar table, under good lighting. In this setting, the diagnosis is frequently obvious with only simple observation and gentle palpation. Examination in lateral position in the usual exam room with poor lighting is inadequate. Lack of tenderness on rectal examination is reassuring that a high and/or deep abscess is not present.
When the diagnosis is not clear, and certainly if the patient has unexplained fever and/or elevated WBC count in conjunction with deep, unexplained rectal pain, pelvic CT is in order. Endorectal ultrasound examination might also show an abnormality, but will be more uncomfortable for the patient and probably less readily available as well.
Anorectal pain, tenderness, and swelling for which there is no good explanation may require urgent or emergent examination under anesthesia. An alternative is to closely monitor the patient and reexamine for progression of signs and symptoms in 24 to 48 hours, but close observation is mandatory. Treatment is emergent not elective and should not be delayed if abscess is suspected.
Diagnosis and Treatment
The treatment of perianal or intersphincteric abscess is surgical drainage. Whether the drainage procedure is done in the office, in the ED, or in the operating room is a judgment that must be made based on the size and location of the abscess, the cooperativeness and willingness of the patient, the skill and experience of the surgeon, and the resources available, such as instruments, lighting, and assistance. As a general rule, incision and drainage should be performed in the operating room unless the abscess is quite small and superficial.
When an abscess is suspected, the incision for drainage is best made over the point of maximal tenderness and swelling. Attempts to identify the presence or location of a perianal or an intersphincteric abscess by exploration and aspiration with an 18-gauge needle are frequently misleading or unrewarding. While it is possible that the abscess may be small and hard to hit with a needle, more often this maneuver fails because the pus is so thick that it does not flow through the needle and cannot be aspirated. Moreover, if one does happen to find the abscess and aspirates most of the pus from it, this will make it harder to locate after an incision is made.
In making an exploratory incision, knowledge of the perianal anatomy and how to identify the sphincters and intersphincteric plane is important. Sometimes, an incision is made and no abscess can be found. This is acceptable and preferable to missing an abscess. Close follow-up in such instances is recommended because a small abscess may have been missed.
Surgical Approach
Perianal abscess, if superficial, small and obvious, may be drained in the office or emergency department under local anesthesia, with or without sedation. 1% lidocaine with epinephrine 1:100,000 or 1:200,000 is infiltrated into the dermis (not the subcutaneous tissue) over and around the abscess. A lanceolate or an elliptical incision oriented either radially or tangentially to the anus is made over the abscess. This incision will remove a segment of overlying skin. Excision of the skin overlying the abscess helps to completely unroof it and drain it adequately (Figure 6). Cruciate incision is both ugly and inadequate and does not provide good drainage. A small wick of moistened plain cotton gauze is placed into the abscess cavity and removed in 48 hours. Iodoform gauze is harsh, painful, and necrosis inducing and in my opinion should never be used. Rayon or polyester-based packing strip should be avoided as well.

FIGURE 6 • Appearance 2 days after incision and drainage of intersphincteric abscess demonstrating good drainage. An ellipse of skin was removed by using a lanceolate incision at time of I&D.
If the abscess is deeper, larger, or more extensive, having expanded laterally in the intersphincteric plane and partially encircled the anal sphincter to form a horseshoe, a different approach is needed. In general, in this situation, one should avoid large or deep radial incisions, which might divide anal sphincter muscle. Tangential or circumferential incisions are preferred. In the case of horseshoe abscess, multiple small incisions are made through which a drain, such as a small Malecot catheter, rather than packing can be placed and secured with suture. Simple packing can be placed alongside the drains and removed in 24 to 48 hours, leaving the Malecot or equivalent drains in place for a much longer period as the abscess cavity closes.
If the patient does not have an acute abscess, but rather has intermittent drainage, the surgical approach is to evaluate the patient under anesthesia, looking for a fistula in ano. Fine silver or lacrimal duct probes are needed. Hydrogen peroxide solution injected through a fine cannula into an external opening can be helpful in identifying an occult internal opening. If a fistula is found, treatment will depend on the depth and characteristics of the fistula. In this situation, prior measurement of the anal sphincter length by careful rectal examination prior to induction of anesthesia can be critical. If there is acute inflammation or an underlying occult abscess, or if sphincter length is unknown, the best approach is to place a seton through the fistula for drainage and allow the inflammation to subside. One should never do a fistulotomy in the face of an acute abscess or without knowing the sphincter length. Sphincter length cannot be determined under anesthesia, but rather only by examination in an awake patient. It is done by palpation of the posterior anal canal with one’s finger and measuring the distance from the levator ring at one’s fingertip to the anal verge. Normal sphincter length is from 2 to 5 cm. One should try to preserve at least two and preferably 2.5 cm of anal sphincter when doing an I&D or fistulotomy.
It is possible for a patient to have recurrent buttock abscesses as a result of unrecognized fistula in ano (Figure 7). If the abscesses are subcutaneous rather than deep (i.e., in the ischiorectal fossa), one should look for an underlying fistula (Table 1).
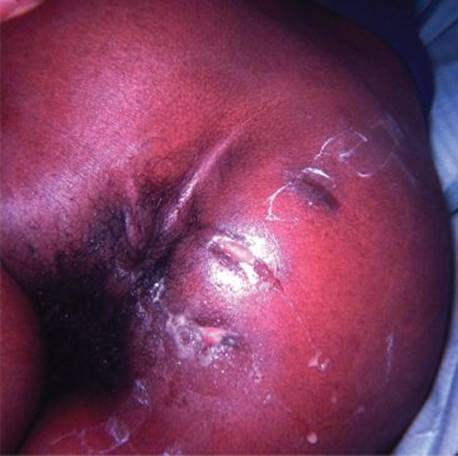
FIGURE 7 • This patient had undergone repeated I&D procedures for buttock abscess before an underlying posterior fistula in ano was sought, found and treated.
TABLE 1. Key Technical Steps and Potential Pitfalls

Special Intraoperative Considerations
The position of the patient on the operating table can be a matter of personal preference. In general, my preference is to do evaluation under anesthesia in the prone position under spinal or caudal anesthesia, unless the patient has a contraindication to this, such as extreme obesity. If general anesthesia is needed in an obese patient, lithotomy position is preferred to avoid the added anesthetic risk of general anesthesia in the prone position. I position the patient prone with hips over the kidney rest, which I elevate several inches prior to flexing the table. Gel pads to support the pelvis and chest are not needed if spinal anesthesia is used unless the patient has a very obese abdomen. Pulling the buttocks apart with 3-inch adhesive tape angled about 30 degrees toward the head improves exposure of the perianal region.
Prep solutions may obscure the skin erythema that provides a clue as to the location of the abscess. Marking the site with permanent skin marker before prepping obviates this problem. If an intersphincteric abscess is suspected, the intersphincteric plane must be identified and opened bluntly to gain access to and drain the abscess. A tangential incision parallel to the sphincter muscle is helps prevent unwittingly dividing muscle unnecessarily.
If an exploratory incision is made and no pus is found, do not suture the wound closed or pack it open. Simply place a dressing over the unclosed wound. If pus is found, culture is not usually helpful in otherwise healthy individuals. Aerobic and anaerobic cultures can be obtained if you have reason to suspect resistant organisms and if the patient has immune compromise, is in poor general health, or appears septic because of high fever and WBC count.
As mentioned above, avoid the use of Iodoform gauze, which has no proven benefit, causes pain, and impairs wound healing. Simple saline- or plain water-moistened plain cotton gauze works quite well.
Postoperative Management
Sitz baths are traditional for comfort and to promote drainage. The initial packing can be left in place for 48 to 72 hours. If the patient has a simple perianal abscess, the packing once removed does not have to be replaced if a small ellipse of skin has been removed by the lanceolate incision because the skin edges will not close prematurely. Antimicrobial therapy can be discontinued after a brief period unless cellulitis is present.
If the abscess is larger, more complex, and deep, it is best to use Malecot or a similar catheter for drainage and to leave it in place for days or weeks. The wound can be irrigated two to three times a day through the drainage tube. The tube can be downsized as the cavity closes. If the wound is superficial but extensive and/or partially circumferential, wound care consisting of shower irrigation and water-moistened plain gauze dressings changed three times a day leads to good healing (Figures 8 and 9).

FIGURE 8 • Appearance of large perianal wound 2 weeks after incision and drainage of superficial horseshoe abscess. Wound care consisted of plain water-moistened gauze dressings changed three times a day.

FIGURE 9 • The wound contracted and healed completely with minimal residual scar.
TAKE HOME POINTS
· Acute anal pain and swelling is not a trivial problem and demands urgent attention.
· Examination under anesthesia should be done if there is any question of occult or complicated abscess.
· Pelvic CT is not usually needed, but is indicated if supralevator abscess is suspected. Failure to aspirate pus through a needle does not mean an abscess is not present.
· Incision should be generous, with removal of overlying skin to promote adequate drainage.
· Do not attempt fistulotomy in the face of acute inflammation; place a seton if a fistula is obvious. Use plain, moist gauze packing and leave initial packing for 48 hours.
· If abscess is large and/or deep, place a Malecot or equivalent drain sutured in place.