Objectives
● The student understands the homeostatic role of the cardiovascular system, the basic principles of cardiovascular transport, and the basic structure and function of the components of the system:
● Defines homeostasis.
● Identifies the major body fluid compartments and states the approximate volume of each.
● Lists 3 conditions, provided by the cardiovascular system, that are essential for regulating the composition of interstitial fluid (i.e., the internal environment).
● Predicts the relative changes in flow through a tube caused by changes in tube length, tube radius, fluid viscosity, and pressure difference.
● Uses the Fick principle to describe convective transport of substances through the CV system and to calculate a tissue’s rate of utilization (or production) of a substance.
● dentifies the chambers and valves of the heart and describes the pathway of blood flow through the heart.
● Defines cardiac output and identifies its 2 determinants.
● Describes the site of initiation and pathway of action potential propagation in the heart.
● States the relationship between ventricular filling and cardiac output (the Starling law of the heart) and describes its importance in the control of cardiac output.
● dentifies the distribution of sympathetic and parasympathetic nerves in the heart and lists the basic effects of these nerves on the heart.
● Lists the 5 factors essential to proper ventricular pumping action.
● Lists the major different types of vessels in a vascular bed and describes the morphological differences among them.
● Describes the basics and functions of the different vessel types.
● dentifies the major mechanisms in vascular resistance control and blood flow distribution.
● Describes the basic composition of the fluid and cellular portions of blood.
Evolution and homeostatic role of the cardiovascular system
All living organisms require outside energy sources to survive. Indeed, Darwin deduced his evolutionary concepts largely on observations of external adaptations that evolved in different organisms to exploit particular unique sources of “food” energy. Clearly one strong evolutionary force has been to maximize the ability to obtain outside energy.
In the big picture of “survival of the fittest,” equally important to obtaining outside energy is making efficient use of it once it is obtained. Therefore, we contend that developing energy-efficient mechanisms to accomplish all internal tasks necessary for successful life has also been a strong evolutionary force and probably applies to all “internal” processes.
In this text, we focus on how the design and operation of the human cardiovascular system has evolved to accomplish its essential tasks with a minimum of energy expenditure.
A 19th-century French physiologist, Claude Bernard (1813-1878), first recognized that all higher organisms actively and constantly strive to prevent the external environment from upsetting the conditions necessary for life within the organism. Thus, the temperature, oxygen concentration, pH, ionic composition, osmolarity, and many other important variables of our internal environment are closely controlled. This process of maintaining the “constancy” of our internal environment has come to be known as homeostasis. To aid in this task, an elaborate material transport network, the cardiovascular system, has evolved.
Three compartments of watery fluids, known collectively as the total body water, account for approximately 60% of body weight in a normal adult. This water is distributed among the intracellular, interstitial, and plasma compartments, as indicated in Figure 1-1. Note that about two- thirds of our body water is contained within cells and communicates with the interstitial fluid across the plasma membranes of cells. Of the fluid that is outside cells (i.e., extracellular fluid), only a small amount, the plasma volume, circulates within the cardiovascular system. Total circulating blood volume is larger than that of blood plasma, as indicated in Figure 11, because blood also contains suspended blood cells that collectively occupy approximately 40% of its volume. However, it is the circulating plasma that directly interacts with the interstitial fluid of body organs across the walls of the capillary vessels.
The interstitial fluid is the immediate environment of individual cells.
(It is the “internal environment” referred to by Bernard.) These cells must draw their nutrients from and release their products into the interstitial fluid. The interstitial fluid cannot, however, be considered a large reservoir for nutrients or a large sink for metabolic products, because its volume is less than half that of the cells that it serves. The well-being of individual cells therefore depends heavily on the homeostatic mechanisms that regulate the composition of the interstitial fluid. This task is accomplished by continuously exposing the interstitial fluid to “fresh” circulating plasma fluid.

Figure 1-1. Major body fluid compartments with average volumes indicated for a normal 70-kg adult human. Total body water is approximately 60% of body weight.
As blood passes through capillaries, solutes exchange between plasma and interstitial fluid by the process of diffusion. The net result of transcapillary diffusion is always that the interstitial fluid tends to take on the composition of the incoming blood. If, for example, potassium ion concentration in the interstitium of a particular skeletal muscle was higher than that in the plasma entering the muscle, then potassium would diffuse into the blood as it passes through the muscle’s capillaries. Because this removes potassium from the interstitial fluid, its potassium ion concentration would decrease. It would stop decreasing when the net movement of potassium into capillaries no longer occurs, that is, when the concentration of the interstitial fluid reaches that of incoming plasma.
Three conditions are essential for this circulatory mechanism to effectively control the composition of the interstitial fluid: (1) there must be adequate blood flow through the tissue capillaries; (2) the chemical composition of the incoming (or arterial) blood must be controlled to be that which is optimal in the interstitial fluid; and (3) diffusion distances between plasma and tissue cells must be short. Figure 1-1 shows how the cardiovascular transport system operates to accomplish these tasks. Diffusional transport within tissues occurs over extremely small distances because no cell in the body is located farther than approximately 10 pm from a capillary. Over such microscopic distances, diffusion is a very rapid process that can move huge quantities of material. Diffusion, however, is a very poor mechanism for moving substances from the capillaries of an organ, such as the lungs, to the capillaries of another organ that may be 1 m or more distant. Consequently, substances are transported between organs by the process of convection, by which the substances easily move along with blood flow because they are either dissolved or contained within blood. The relative distances involved in cardiovascular transport are not well illustrated in Figure 1-1. If the figure was drawn to scale, with 1 inch representing the distance from capillaries to cells within a calf muscle, then the capillaries in the lungs would have to be located about 15 miles away!
Overall design of the cardiovascular system
The overall functional arrangement of the cardiovascular system is illustrated in Figure 1-2. Because a functional rather than an anatomical viewpoint is expressed in this figure, the role of heart appears in 3 places: as the right heart pump, as the left heart pump, and as the heart muscle tissue. It is common practice to view the cardiovascular system as (1) the pulmonary circulation, composed of the right heart pump and the lungs, and (2) the systemic circulation, in which the left heart pump supplies blood to the systemic organs (all structures except the gas exchange portion of the lungs). The pulmonary and systemic circulations are arranged in series, that is, one after the other. Consequently, both the right and left hearts must pump an identical volume of blood per minute. This amount is called the cardiac output.
As indicated in Figure 1-2, most systemic organs are functionally arranged in parallel (i.e., side by side) within the cardiovascular system.
There are 2 important consequences of this parallel arrangement. First, nearly all systemic organs receive blood of identical composition—that which has just left the lungs and is known as arterial blood. Second, the flow through any one of the systemic organs can be controlled independently of the flow through the other organs. Thus, for example, the cardiovascular response to whole-body exercise can involve increased blood flow through some organs, decreased blood flow through others, and unchanged blood flow through yet others.
Many of the organs in the body help perform the task of continually reconditioning the blood circulating in the cardiovascular system. Key roles are played by organs, such as the lungs, that communicate with the external environment. As is evident from the arrangement shown in Figure 1-2, any blood that has just passed through a systemic organ returns to the right heart and is pumped through the lungs, where oxygen and carbon dioxide are exchanged. Thus, the blood’s gas composition is always reconditioned immediately after leaving a systemic organ.
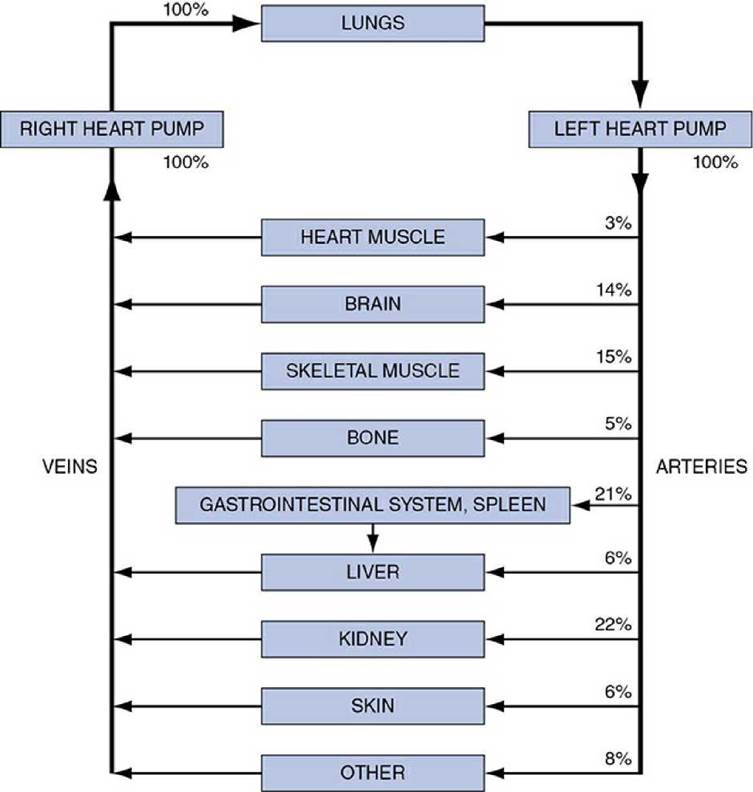
Figure 1-2. Cardiovascular circuitry, indicating the percentage distribution of cardiac output to various organ systems in a resting individual.
Like the lungs, many of the systemic organs also serve to recondition the composition of blood, although the flow circuitry precludes their doing so each time the blood completes a single circuit. The kidneys, for example, continually adjust the electrolyte composition of the blood passing through them. Because the blood conditioned by the kidneys mixes freely with all the circulating blood and because electrolytes and water freely pass through most capillary walls, the kidneys control the electrolyte balance of the entire internal environment. To achieve this, it is necessary that a given unit of blood pass often through the kidneys. In fact, the kidneys normally receive about one-fifth of the cardiac output under resting conditions. This greatly exceeds the amount of flow that is necessary to supply the nutrient needs of the renal tissue. This situation is common to organs that have a blood-conditioning function.
Blood-conditioning organs can also withstand, at least temporarily, severe reduction of blood flow. Skin, for example, can easily tolerate a large reduction in blood flow when it is necessary to conserve body heat. Most of the large abdominal organs also fall into this category. The reason is simply that because of their blood-conditioning functions, their normal blood flow is far in excess of that necessary to maintain their basal metabolic needs.
The brain, heart muscle, and skeletal muscles typify organs in which blood flows solely to supply the metabolic needs of the tissue. They do not recondition the blood for the benefit of any other organ. Normally, the blood flow to the brain and the heart muscle is only slightly greater than that required for their metabolism; hence, they do not tolerate blood flow interruptions well. Unconsciousness can occur within a few seconds after stoppage of cerebral flow, and permanent brain damage can occur in as little as 4 minutes without flow. Similarly, the heart muscle (myocardium) normally consumes approximately 75% of the oxygen supplied to it, and the heart’s pumping ability begins to deteriorate within beats of a coronary flow interruption. As we shall see later, the task of providing adequate blood flow to the brain and the heart muscle receives a high priority in the overall operation of the cardiovascular system.
Cardiac muscle must do physical work to move blood through the circulatory system. Note in Figure 1-2 that the cardiac muscle itself requires only about 3% of all the blood it is pumping to sustain its own operation. The clear implication is that the heart has evolved into a very efficient pump.
Within any given tissue, the blood flow required to maintain local homeostasis is directly related to its current cellular metabolic rate. Under challenges of daily life, metabolic activity of many individual organs can change dramatically from situation to situation. For example, metabolic rate of maximally active skeletal muscle can be 50 times that of its inactive (resting) rate. Thus, it is essential for the cardiovascular system to rapidly adapt to ever-changing needs in the body. As far as the heart is concerned, the bottom line is how much blood flow it must produce in different situations regardless of where that total flow is directed. Cardiac output in a resting human adult is about 5 to 6 L/min (80 gallons/h, 2000 gallons/day!) and can increase to 3 to 4 times that amount during maximal exercise. Presumably, the cardiovascular system has evolved to efficiently operate over that range.
The basic physics of blood flow
One of the most important keys to comprehending how the cardiovascular system operates is to have a thorough understanding of the relationship among the physical factors that determine the rate of fluid flow through a tubular vessel.
The tube depicted in Figure 1-3 might represent a segment of any vessel in the body. It has a certain length (L) and a certain internal radius ( r) through which blood flows. Fluid flows through the tube only when the pressures in the fluid at the inlet and outlet ends ( P i and P o) are unequal, that is, when there is a pressure difference (Д P) between the ends. Pressure differences supply the driving force for flow. Because friction develops between the moving fluid and the stationary walls of a tube, vessels tend to resist fluid movement through them. This vascular resistance is a measure of how difficult it is to make fluid flow through the tube, that is, how much of a pressure difference it takes to cause a certain flow. The all-important relationship among flow, pressure difference, and resistance is described by the basic flow equation as follows: 
or
![]()
![]()
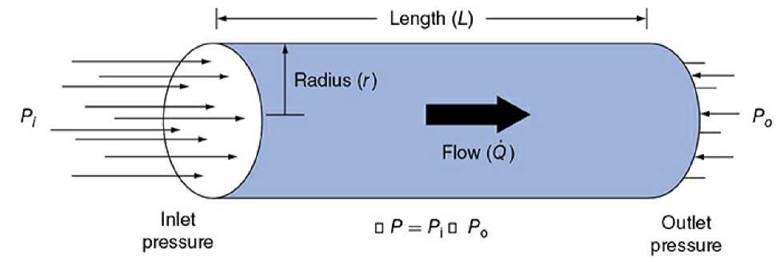
Figure 1-3. Factors influencing fluid flow through a tube.
The basic flow equation may be applied not only to a single tube but also to complex networks of tubes, for example, the vascular bed of an organ or the entire systemic system. The flow through the brain, for example, is determined by the difference in pressure between cerebral arteries and veins divided by the overall resistance to flow through the vessels in the cerebral vascular bed. It should be evident from the basic flow equation that there are only 2 ways in which blood flow through any organ can be changed: (1) by changing the pressure difference across its vascular bed or (2) by changing its vascular resistance. Most often, it is changes in an organ’s vascular resistance that cause the flow through the organ to change.
From the work of the French physician Jean Leonard Marie Poiseuille (1799-1869), who performed experiments on fluid flow through small glass capillary tubes, it is known that the resistance to flow through a cylindrical tube depends on several factors, including the radius and length of the tube and the viscosity of the fluid flowing through it. These factors influence resistance to flow as follows:
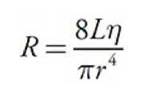
where r = inside radius of the tube, L = tube length, and η = fluid viscosity.
Note especially that the internal radius of the tube is raised to the fourth power in this equation. Thus, even small changes in the internal radius of a tube have a huge influence on its resistance to flow. For example, halving the inside radius of a tube will increase its resistance to flow by 16-fold.
The preceding 2 equations may be combined into one expression known as the Poiseuille equation, which includes all the terms that influence flow through a cylindrical vessel:
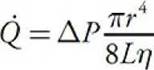
Again, note that flow occurs only when a pressure difference exists. (If A P = 0, then flow = 0.) It is not surprising then that arterial blood pressure is an extremely important and carefully regulated cardiovascular variable. Also note once again that for any given pressure difference, tube radius has a very large influence on the flow through a tube. It is logical, therefore, that organ blood flows are regulated primarily through changes in the radii of vessels within organs. Although vessel length and blood viscosity are factors that influence vascular resistance, they are not variables that can be easily manipulated for the purpose of moment-to- moment control of blood flow.
In regard to the overall cardiovascular system, as depicted in Figures 1-1 and 1-2, one can conclude that blood flows through the vessels within an organ only because a pressure difference exists between the blood in the arteries supplying the organ and the veins draining it. The primary job of the heart pump is to keep the pressure within arteries higher than that within veins. Normally, the average pressure in systemic arteries is approximately 100 mm Hg, and the average pressure in systemic veins is approximately 0 mm Hg.
Therefore, because the pressure difference (A P) is nearly identical across all systemic organs, cardiac output is distributed among the various systemic organs, primarily on the basis of their individual resistances to flow. Because blood preferentially flows along paths of least resistance, organs with relatively low resistance naturally receive relatively high flow.
Material transport by blood flow
Substances are carried between organs within the cardiovascular system by the process of convective transport, the simple process of being swept along with the flow of the blood in which they are contained. The rate at which a substance (X) is transported by this process depends solely on the concentration of the substance in the blood and the blood flow rate.
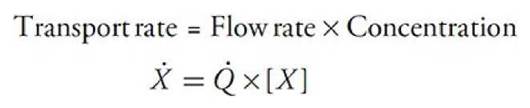
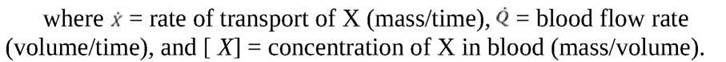
It is evident from the preceding equation that only 2 methods are available for altering the rate at which a substance is carried to an organ: (1) a change in the blood flow rate through the organ or (2) a change in the arterial blood concentration of the substance. The preceding equation might be used, for example, to calculate how much oxygen is carried to a certain skeletal muscle each minute. Note, however, that this calculation would not indicate whether the muscle actually used the oxygen carried to it.
The Fick Principle
One can extend the convective transport principle to calculate the rate at which a substance is being removed from (or added to) the blood as it passes through an organ. To do so, one must simultaneously consider the rate at which the substance is entering the organ in the arterial blood and the rate at which the substance is leaving the organ in the venous blood. The basic logic is simple. For example, if something goes into an organ in arterial blood and does not come out on the other side in venous blood, it must have left the blood and entered the tissue within the organ. This concept is referred to as the Fick principle (Adolf Fick, a German physician, 1829-1901) and may be formally stated as follows:
![]()

stable situation wherein nothing (including the substance’s tissue concentration) is changing with time. Therefore, in the steady state, the rate of the substance’s loss from blood within a tissue must equal its rate of metabolism within that tissue.
The heart
Pumping Action
The heart lies in the center of the thoracic cavity and is suspended by its attachments to the great vessels within a thin fibrous sac called the pericardium. A small amount of fluid in the sac lubricates the surface of the heart and allows it to move freely during contraction and relaxation. Blood flow through all organs is passive and occurs only because arterial pressure is kept higher than venous pressure by the pumping action of the heart. The right heart pump provides the energy necessary to move blood through the pulmonary vessels, and the left heart pump provides the energy to move blood through the systemic organs.
The pathway of blood flow through the chambers of the heart is indicated in Figure 1-4. Venous blood returns from the systemic organs to the right atrium via the superior and inferior venae cavae. This “venous” blood is deficient in oxygen because it has just passed through systemic organs that all extract oxygen from blood for their metabolism. It then passes through the tricuspid valve into the right ventricle and from there it is pumped through the pulmonic valve into the pulmonary circulation via the pulmonary arteries. Within the capillaries of the lung, blood is “reoxygenated” by exposure to oxygen-rich inspired air. Oxygenated pulmonary venous blood flows in pulmonary veins to the left atrium and passes through the mitral valve into the left ventricle. From there it is pumped through the aortic valve into the aorta to be distributed to the systemic organs.

Figure 1-4. Pathway of blood flow through the heart.
Although the gross anatomy of the right heart pump is somewhat different from that of the left heart pump, the pumping principles are identical. Each pump consists of a ventricle, which is a closed chamber surrounded by a muscular wall, as illustrated in Figure 1-5. The valves are structurally designed to allow flow in only one direction and passively open and close in response to the direction of the pressure differences across them. Ventricular pumping action occurs because the volume of the intraventricular chamber is cyclically changed by rhythmic and synchronized contraction and relaxation of the individual cardiac muscle cells that lie in a circumferential orientation within the ventricular wall. 2
When the ventricular muscle cells are contracting, they generate a circumferential tension in the ventricular walls that causes the pressure within the chamber to increase. As soon as the ventricular pressure exceeds the pressure in the pulmonary artery (right pump) or aorta (left pump), blood is forced out of the chamber through the outlet valve, as shown in Figure 1-5. This phase of the cardiac cycle during which the ventricular muscle cells are contracting is called systole. Because the pressure is higher in the ventricle than in the atrium during systole, the inlet or atrioventricular (AV) valve is closed. When the ventricular muscle cells relax, the pressure in the ventricle falls below that in the atrium, the AV valve opens, and the ventricle refills with blood, as shown on the right side in Figure 1-5. This portion of the cardiac cycle is called diastole. The outlet valve is closed during diastole because arterial pressure is greater than intraventricular pressure. After the period of diastolic filling, the systolic phase of a new cardiac cycle is initiated.

Figure 1-5. Ventricular pumping action.
The amount of blood pumped per minute from each ventricle (the cardiac output, CO) is determined by the volume of blood ejected per beat (the stroke volume, SV) and the number of heartbeats per minute (the heart rate, HR) as follows:
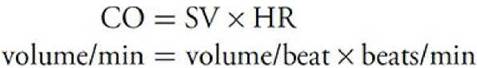
It should be evident from this relationship that all influences on cardiac output must act through changes in either the heart rate or the stroke volume.
An important implication of the above is that the volume of blood that the ventricle pumps with each heartbeat (i.e., the stroke volume, SV) must equal the blood volume inside the ventricle at the end of diastole (end- diastolic volume, EDV) minus ventricular volume at the end of systole (end-systolic volume, ESV). That is,
![]()
Thus, stroke volume can only be changed by changes in EDV and/or ESV. The implication for the bigger picture is that cardiac output can only be changed by changes in HR, EDV, and/or ESV.
Cardiac Excitation
Efficient pumping action of the heart requires a precise coordination of the contraction of millions of individual cardiac muscle cells. Contraction of each cell is triggered when an electrical excitatory impulse ( action potential) sweeps over its membrane. Proper coordination of the contractile activity of the individual cardiac muscle cells is achieved primarily by the conduction of action potentials from one cell to the next via gap junctions that connect all cells of the heart into a functional syncytium (i.e., acting as one synchronous unit). In addition, muscle cells in certain areas of the heart are specifically adapted to control the frequency of cardiac excitation, the pathway of conduction, and the rate of the impulse propagation through various regions of the heart. The major components of this specialized excitation and conduction system are shown in Figure 1-6. These include the sinoatrial node (SA node), the atrioventricular node (AV node), the bundle of His, and the right and left bundle branches made up of specialized cells called Purkinje fibers.
The SA node contains specialized cells that normally function as the heart’s pacemaker and initiate the action potential that is conducted through the heart. The AV node contains slowly conducting cells that normally function to create a slight delay between atrial contraction and ventricular contraction. The Purkinje fibers are specialized for rapid conduction and ensure that all ventricular cells contract at nearly the same instant. The overall message is that HR is normally controlled by the electrical activity of the SA nodal cells. The rest of the conduction system ensures that all the rest of the cells in the heart follow along in proper lockstep for efficient pumping action.
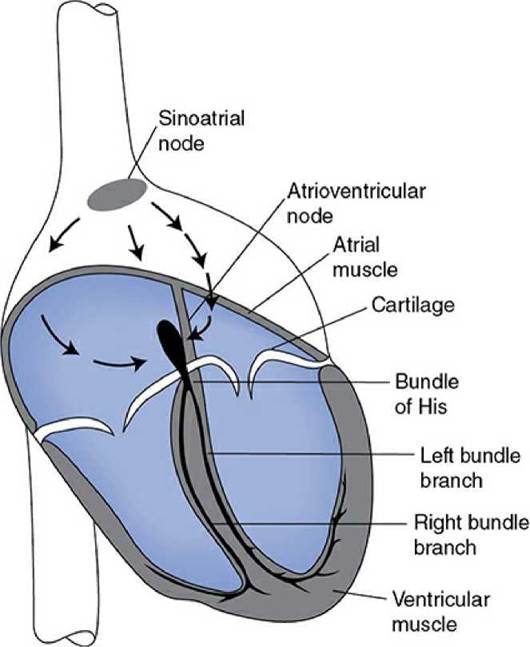
Figure 1-6. Electrical conduction system of the heart.
Control of Cardiac Output
Autonomic neural influences
Although the heart can inherently beat on its own, cardiac function can be influenced profoundly by neural inputs from both the sympathetic and parasympathetic divisions of the autonomic nervous system. These inputs allow us to modify cardiac pumping as is appropriate to meet changing homeostatic needs of the body. All portions of the heart are richly innervated by adrenergic sympathetic fibers. When active, these sympathetic nerves release norepinephrine (noradrenaline) on cardiac cells. Norepinephrine interacts with β1-adrenergic receptors on cardiac muscle cells to increase the heart rate, increase the action potential conduction velocity, and increase the force of contraction and rates of contraction and relaxation. Overall, sympathetic activation acts to increase cardiac pumping.
Cholinergic parasympathetic nerve fibers travel to the heart via the vagus nerve and innervate the SA node, the AV node, and the atrial muscle. When active, these parasympathetic nerves release acetylcholine on cardiac muscle cells. Acetylcholine interacts with muscarinic receptors on cardiac muscle cells to decrease the heart rate (SA node) and decrease the action potential conduction velocity (AV node). Parasympathetic nerves may also act to decrease the force of contraction of atrial (not ventricular) muscle cells. Overall, parasympathetic activation acts to decrease cardiac pumping. Usually, an increase in parasympathetic nerve activity is accompanied by a decrease in sympathetic nerve activity, and vice versa.
Diastolic filling: the starling law of the heart
One of the most fundamental causes of variations in stroke volume was described by William Howell in 1884 and by Otto Frank in 1894 and formally stated by E. H. Starling in 1918. These investigators demonstrated that, with other factors being equal, if cardiac filling increases during diastole, the volume ejected during systole also increases. As a consequence, and as illustrated in Figure 1-7, stroke volume increases nearly in proportion to increases in end-diastolic volume. This phenomenon is commonly referred to as the Starling law of the heart. In a subsequent chapter, we will describe how the Starling law is a direct consequence of the intrinsic mechanical properties of cardiac muscle cells. However, knowing the mechanisms behind the Starling law is not ultimately as important as appreciating its consequences. The primary consequence is that stroke volume (and therefore cardiac output) is strongly influenced by cardiac filling during diastole. Therefore, we shall later pay particular attention to the factors that affect cardiac filling and how they participate in the normal regulation of cardiac output.
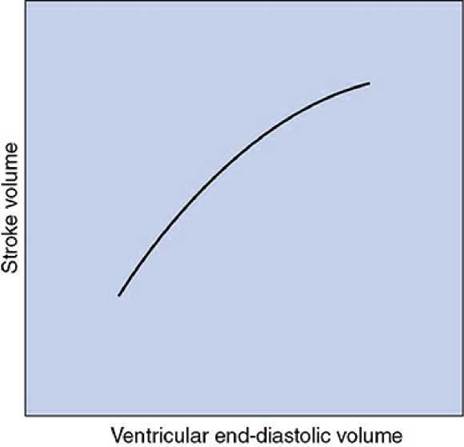
Figure 1-7. The Starling law of the heart.
Requirements for Effective Operation
For effective efficient ventricular pumping action, the heart must be functioning properly in 5 basic respects:
1. The contractions of individual cardiac muscle cells must occur at regular intervals and be synchronized (not arrhythmic).
2. The valves must open fully (not stenotic).
3. The valves must not leak (not insufficient or regurgitant).
4. The muscle contractions must be forceful (not failing).
5. The ventricles must fill adequately during diastole.
In the subsequent chapters, we will study in detail how these requirements are met in the normal heart. Moreover, we will describe how failures in any of these respects lead to distinctly different, clinically relevant, pathologies and symptoms.
The vasculature
Blood that is ejected into the aorta by the left heart passes consecutively through many different types of vessels before it returns to the right heart. As illustrated in Figure 1-8, the major vessel classifications are arteries,
arterioles, capillaries, venules, and veins. These consecutive vascular segments are distinguished from one another by differences in their physical dimensions, morphological characteristics, and function. One thing that all these vessels have in common is that they are lined with a contiguous single layer of endothelial cells. In fact, this is true for the entire circulatory system including the heart chambers and even the valve leaflets.
Vessel Characteristics
Some representative physical characteristics of these major vessel types are shown in Figure 1-8. It should be realized, however, that the vascular bed is a continuum and that the transition from one type of vascular segment to another does not occur abruptly. The total cross-sectional area through which blood flows at any particular level in the vascular system is equal to the sum of the cross-sectional areas of all the individual vessels arranged in parallel at that level. The number and total cross-sectional area values presented in Figure 1-8 are estimates for the entire systemic circulation.
Arteries are thick-walled vessels that contain, in addition to some smooth muscle, a large component of elastin and collagen fibers. Primarily because of the elastin fibers, which can stretch to twice their unloaded length, arteries can expand under increased pressure to accept and temporarily store some of the blood ejected by the heart during systole and then, by passive recoil, supply this blood to the organs downstream during diastole. The aorta is the largest artery and has an internal (luminal) diameter of approximately 25 mm. Arterial diameter decreases with each consecutive branching, and the smallest arteries have diameters of approximately 0.1 mm. The consecutive arterial branching pattern causes an exponential increase in arterial numbers. Thus, although individual vessels get progressively smaller, the total cross-sectional area available for blood flow within the arterial system increases to several fold that in the aorta. Arteries are often referred to as conduit vessels because they have relatively low and unchanging resistance to flow.
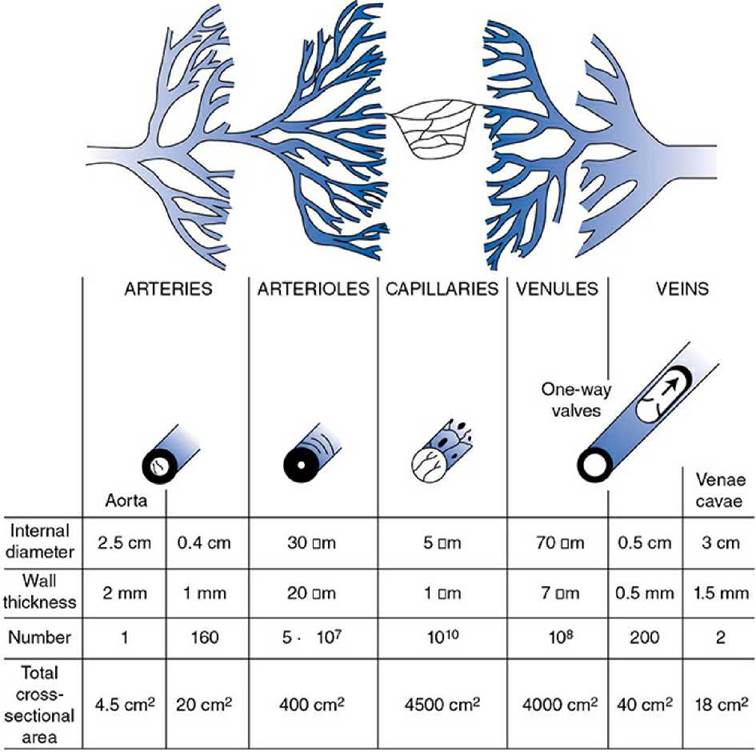
Figure 1-8. Structural characteristics of the peripheral vascular system.
Arterioles are smaller and structured differently than arteries. In proportion to lumen size, arterioles have much thicker walls with more smooth muscle and less elastic material than do arteries. Because arterioles are so muscular, their diameters can be actively changed to regulate the blood flow through peripheral organs. Despite their minute size, arterioles are so numerous that in parallel their collective cross-sectional area is much larger than that at any level in arteries. Arterioles are often referred to as resistance vessels because of their high and changeable resistance, which regulates peripheral blood flow through individual organs.
Capillaries are the smallest vessels in the vasculature. In fact, red blood cells with diameters of 7 μm must deform to pass through them. The capillary wall consists of a single layer of endothelial cells that separates the blood from the interstitial fluid by only approximately 1 pm. Capillaries contain no smooth muscle and thus lack the ability to change their diameters actively. They are so numerous that the total collective cross-sectional area of all the capillaries in systemic organs is more than 1000 times that of the root of the aorta. Given that capillaries are approximately 0.5 mm in length, the total surface area available for exchange of material between blood and interstitial fluid can be calculated to exceed 100 m 2. For obvious reasons, capillaries are viewed as the exchange vessels of the cardiovascular system. In addition to the transcapillary diffusion of solutes that occurs across these vessel walls, there can sometimes be net movements of fluid (volume) into and/or out of capillaries. For example, tissue swelling ( edema) is a result of net fluid movement from plasma into the interstitial space.
After leaving capillaries, blood is collected in venules and veins and returned to the heart. Venous vessels have very thin walls in proportion to their diameters. Their walls contain smooth muscle, and their diameters can actively change. Because of their thin walls, venous vessels are quite distensible. Therefore, their diameters change passively in response to small changes in transmural distending pressure (i.e., the difference between the internal and external pressures across the vessel wall). Venous vessels, especially the larger ones, also have one-way valves that prevent reverse flow. As will be discussed later, these valves are especially important in the cardiovascular system’s operation during standing and during exercise. It turns out that peripheral venules and veins normally contain more than 50% of the total blood volume. Consequently, they are commonly thought of as the capacitance vessels. More importantly, changes in venous volume greatly influence cardiac filling and therefore cardiac pumping. Thus, peripheral veins actually play an extremely important role in controlling cardiac output.
Control of Blood Vessels
Blood flow through individual vascular beds is profoundly influenced by changes in the activity of sympathetic nerves innervating arterioles. These nerves release norepinephrine at their endings that interacts with a - adrenergic receptors on the smooth muscle cells to cause contraction and thus arteriolar constriction. The reduction in arteriolar diameter increases vascular resistance and decreases blood flow. These neural fibers provide the most important means of reflex control of vascular resistance and organ blood flow.
Arteriolar smooth muscle is also very responsive to changes in the local chemical conditions within an organ that accompany changes in the metabolic rate of the organ. For reasons to be discussed later, increased tissue metabolic rate leads to arteriolar dilation and increased tissue blood flow.
Venules and veins are also richly innervated by sympathetic nerves and constrict when these nerves are activated. The mechanism is the same as that involved with arterioles. Thus, increased sympathetic nerve activity is accompanied by decreased venous volume. The importance of this phenomenon is that venous constriction tends to increase cardiac filling and therefore cardiac output via the Starling law of the heart.
To the best of our knowledge, there is no important neural or local metabolic control of either arterial or capillary vessel tone or diameter.
Overall Vascular Function
In essence, the bulk of the vascular system is simply the network of “pipes” necessary to route blood flow from the heart through capillary beds in organs throughout the body and then collect it again to return it to the heart. Because blood is a viscous fluid, there is an unavoidable energy loss (to heat via fluid friction) as it flows through any vessel. Thus, there is an energy cost to just distributing the blood throughout the body. This energy loss as blood moves through the vasculature is important because it determines how much work the heart must do to produce that flow in the first place.
There are many possible plumbing schemes (e.g., various combinations of vessels of different diameters, lengths, and branching patterns) that could accomplish the goal of distributing blood to capillary beds throughout the body. However, some would do so with less frictional energy loss than others. We contend that the vascular system has evolved to distribute the cardiac output with minimal energy loss in the process.
Blood
Blood is a complex fluid that serves as the medium for transporting substances between the tissues of the body and performs a host of other functions as well. Normally, approximately 40% of the volume of whole blood is occupied by blood cells that are suspended in the watery fluid, plasma, which accounts for the rest of the volume. The fraction of blood volume occupied by cells is termed as the hematocrit, a clinically important parameter.
Hematocrit = Cell volume/Totalblood volume
One of the reasons that a person’s hematocrit is clinically relevant is that the viscosity of blood increases dramatically with increases in its hematocrit. Recall that fluid viscosity is one physical factor that affects the flow through a tube. Other factors equal, the higher the blood viscosity, the more work the heart has to do to produce any given flow through the vasculature.
Blood Cells
Blood contains 3 general types of “formed elements”: red cells, white cells, and platelets (see Appendix A). All are formed in bone marrow from a common stem cell. Red cells are by far the most abundant. They are specialized to carry oxygen from the lungs to other tissues by binding oxygen to hemoglobin, an iron-containing heme protein contained within red blood cells. Because of the presence of hemoglobin, blood can transport 40 to 50 times the amount of oxygen that plasma alone could carry. In addition, the hydrogen ion buffering capacity of hemoglobin is vitally important to the blood’s capacity to transport carbon dioxide.
A small, but important, fraction of the cells in blood is white cells or leukocytes. Leukocytes are involved in immune processes. Appendix A gives more information on the types and function of leukocytes. Platelets are small cell fragments that are important in the blood-clotting process.
Plasma
Plasma is the liquid component of blood and, as indicated in Appendix B, is a complex solution of electrolytes and proteins. Serum is the fluid obtained from a blood sample after it has been allowed to clot. For all practical purposes, the composition of serum is identical to that of plasma except that it contains none of the clotting proteins.
Inorganic electrolytes (inorganic ions such as sodium, potassium, chloride, and bicarbonate) are the most concentrated solutes in plasma. Of these, sodium and chloride are by far the most abundant and, therefore, are primarily responsible for plasma’s normal osmolarity of approximately 300 mOsm/L. To a first approximation, the “stock” of the plasma soup is a 150-mM solution of sodium chloride. Such a solution is called “isotonic saline” and has many clinical uses as a fluid that is compatible with cells.
Plasma normally contains many different proteins. Most plasma proteins can be classified as albumins, globulins, or fibrinogen on the basis of different physical and chemical characteristics used to separate them. More than 100 distinct plasma proteins have been identified and each presumably serves some specific function. Many plasma proteins are involved in blood clotting or immune/defense reactions. Many others are important carrier proteins for a variety of substances including fatty acids, iron, copper, vitamin D, and certain hormones.
Proteins do not readily cross capillary walls and, in general, their plasma concentrations are much higher than their concentrations in the interstitial fluid. As will be discussed, plasma proteins play an important osmotic role in transcapillary fluid movement and consequently in the distribution of extracellular volume between the plasma and interstitial compartments. Albumin plays an especially strong role in this regard simply because it is by far the most abundant of the plasma proteins.
Plasma also serves as the vehicle for transporting nutrients and waste products. Thus, a plasma sample contains many small organic molecules such as glucose, amino acids, urea, creatinine, and uric acid whose measured values are useful in clinical diagnosis.
Perspectives
In this first chapter, we have argued that maintaining bodily homeostasis is the bottom-line task of the cardiovascular system. To maintain homeostasis in any tissue in any given situation, that tissue must receive a blood flow through its capillaries that is matched to support the local current metabolic needs of that tissue. Adequate arterial pressure is necessary to produce tissue blood flow in the first place but arterial pressure is only one factor in achieving adequate tissue blood flow. Constant arterial pressure by itself does not ensure that there will be homeostasis throughout the body. What constant arterial pressure does do is allow an individual organ to control its own blood flow by varying the local resistance to blood flow according to its current metabolic needs. Moreover, this local control allows any organ to regulate its own flow without disturbing the flows through other organs. At this juncture we would also like to draw the reader’s attention to Appendix C, which is a shorthand compilation of many of the key cardiovascular relationships that we have and will encounter in due course.
Key concepts
The primary role of the cardiovascular system is to maintain homeostasis in the interstitial fluid.
The physical law that governs cardiovascular operation is that flow through any segment is equal to pressure difference across that segment divided by its resistance to flow, that is,![]() .
.
The rate of transport of a substance within the blood (X) is a function of its concentration in the blood [X] and the blood flow rate, that is,![]() .
.
The heart pumps blood by rhythmically filling and ejecting blood from the ventricular chambers that are served by passive one-way inlet and outlet valves.
Cardiac output (CO) is a function of the heart rate (HR) and stroke volume (SV), that is,![]()
Changes in heart rate and stroke volume (and therefore cardiac output) can be accomplished by alterations in ventricular filling and by alterations in autonomic nerve activity to the heart.
Blood flow through individual organs is regulated by changes in the diameter of their arterioles.
Changes in arteriolar diameter can be accomplished by alterations in sympathetic nerve activity and by variations in local conditions.
Blood is a complex suspension of red cells, white cells, and platelets in plasma that is ideally suited to carry gases, salts, nutrients, and waste molecules throughout the system.
Study questions
1-1. Which organ in the body always receives the most blood flow?
1-2. Whenever skeletal muscle blood flow increases, blood flow to other organs must decrease. True or false?
1-3. When a heart valve does not close properly, a sound called a “murmur” can often be detected as the valve leaks. Would you expect a leaky aortic valve to cause a systolic or diastolic murmur?
1-4. Slowing of action potential conduction through the AV node will slow the heart rate. True or false?
1-5. Suppose the diameters of the vessels within an organ increase by 10%. Other factors equal, how would this affect the
a. resistance to blood flow through the organ?
b. blood flow through the organ?
1-6. The pressure in the aorta is normally about 100 mm Hg, whereas that in the pulmonary artery is normally about 15 mm Hg. A few of your fellow students offer the following alterative hypotheses about why this might be so:
a. The right heart pumps less blood than the left heart.
b. The right heart rate is slower than the left heart rate.
c. The right ventricle is less muscular than the left ventricle.
d. The pulmonary vascular bed has less resistance than the systemic bed.
e. The stroke volume of the right heart is less than that of the left heart.
f. It must be genetics.
Which of their suggestions is (are) correct?
1-7. Usually, an individual who has lost a significant amount of blood is weak and does not reason very clearly. Why would blood loss have these effects?
1-8. What direct cardiovascular consequences would you expect from an intravenous injection of norepinephrine?
1-9. What direct cardiovascular effects would you expect from an intravenous injection of a drug that stimulates a -adrenergic receptors but not β-adrenergic receptors ?
[-10. Individuals with high arterial blood pressure (hypertension) are often treated with drugs that block β-adrenergic receptors. What is a rationale for such treatment?
[-11. The clinical laboratory reports a serum sodium ion value of 140mEq/L in a blood sample you have taken from a patient. What does this tell you about the sodium ion concentration in plasma, in interstitial fluid, and in intracellular fluid?
[-12. Explain how it is that the water flow into your kitchen sink changes when you turn the handle on its faucet.
[-13. A common “side effect” of β-blocker therapy is decreased exercise tolerance. Why is this not surprising?
[-14. You need to determine the correct dose of an IV drug that distributes only within the extracellular space. Which of the following values would be the closest estimate of the extracellular fluid volume of a healthy young adult male weighing 100 kg (220 lb)?
a. 3 L
b. 5 L
c. 8 L
d. 10 L
e. 20 L
[-15. Determine the rate of glucose uptake by an exercising skeletal muscle ( ) from the following data:
Arterial blood glucose concentration, [G] a = 50 mg/100 mL Muscle venous blood glucose concentration, [G] v = 30 mg/100 mL
Muscle blood flow![]()
[-16. The Fick principle implies that doubling the flow through an organ will necessarily double the organ’s rate of metabolism (or production) of a substance. True or False?
[-17. Five requirements for normal cardiac pumping action were listed in this chapter. Recall that CO = HR x (EDV - ESV). Use this as a basis for explaining in detail why a lack of each of the requirements would adversely affect CO.
1 Although pressure is most correctly expressed in units of force per unit area, it is customary to express pressures within the cardiovascular system in millimeters of mercury. For example, mean arterial pressure may be said to be 100 mm Hg because it is same as the pressure existing at the bottom of a mercury column 100 mm high. All cardiovascular pressures are expressed relative to atmospheric pressure, which is approximately 760 mm Hg.
2 The basic pumping principle of the heart has a very long evolutionary history. Eons before mammals evolved, bivalve mollusks were using the same principle to pump water through themselves to harvest food energy from microscopic organisms living in that water.