I. TRAUMATIC NECK PAIN WITHOUT ARM PAIN
A. Introduction. Trauma to the neck secondary to a motor vehicle accident, work-related injury, or athletic injury is a common cause of musculoskeletal neck pain. In the vast majority of patients, post-traumatic neck pain is a self-limited problem that is not serious.
B. Etiology. Straining of anterior/posterior cervical muscles and tendons is the mechanism of pain for most post-traumatic neck pain syndromes. The most common cause in clinical practice is vehicular accidents with hyperextension/flexion to the neck (whiplash). Altercations, athletic injuries (especially football), and lifting/tugging work injuries also occur.
C. Evaluation.
1. History and physical examination. The primary complaints are post-traumatic neck pain and neck stiffness. The paracervical muscles are tender with limitation of motion, spinous process point tenderness may be present and there may be some associated interscapular pain and headache. Complaints of patchy arm numbness are occasionally reported but the neurologic exam is normal for the vast majority of patients.
2. Radiographs.
a. Plain X-rays rule out most fractures and ligamentous instability. In the under-40 age group, the most common finding is loss of the lordotic curve from muscle spasm. In the over-40 age group, X-rays often show degenerative changes such as narrowed disc spaces and osteophyte (bone spur) formation. The accident is not the cause of these X-ray changes but certainly these changes can predispose the patient to more pain than a normal spine.
b. CT scan/MRI scan. Any clinical or radiographic evidence for acute fracture, subluxation (instability), or spinal cord injury requires a thorough evaluation including a cervical CT scan, consultation with a spine specialist and, more often than not, a cervical MRI scan.
D. Referral.
1. First 2 to 3 weeks (medicate and wait).
a. Soft collar. Post-traumatic neck pain will usually subside on its own over a week or. A narrow soft cervical collar can be helpful in taking the weight of the head off the neck and transferring it to the shoulders. The collar should not be so tall that it forces that patient into hyperextension, which is uncomfortable.
b. Medication. Over the counter nonsteroidal anti-inflammatory medication (ibuprofen) with/without acetaminophen is the ideal analgesic. Other analgesics, such as propoxyphene, codeine, or codeine analogs, are acceptable but no schedule-3 narcotics, such as oxycodone, demerol, or morphine, should be used. Muscle relaxants such as Robaxin (methocarbamol) 500 mg P.O. every 6 to 8 hours, Flexeril (cyclobenzaprine) 10 mg P.O. three times a day, or Parafon Forte (chlorzoxazone) 500 mg P.O. every 6 to 8 hours can help. Do not use benzodiazepines due to the abuse potential. In the patient whose stomach is sensitive to nonsteroidal medication, an evening dose of an H-2 receptor blocker such as cimetidine 300 to 600 mg P.O. can help prevent gastritis.
c. Time-off from work. Desk-bound workers with mild to moderate neck pain can work, and most ambitious people are able to function. Heavy laborers may benefit from light duty or 1 to 2 weeks off work. Beware of patients who exhibit symptom magnification and functional overlay due for purposes of secondary gain (worker’s compensation and litigation). They have the tendency to abuse time-off work. In these scenarios, early referral to a physical medicine and rehabilitation specialist who can scientifically assess for malingering may be helpful.
2. Weeks 3 to 6 if pain still present.
a. Physical therapy. If the neck pain does not subside after 2 weeks, physical therapy—heat, ultrasound, massage, and transcutaneous electrical nerve stimulation (TENS)—is reasonable.
b. Pain clinic. Trigger point injections of anesthetic/steroid can be helpful but are probably best scheduled after evaluation by a spine specialist.
3. After 6 to 8 weeks. When neck pain persists after 6 to 8 weeks, despite rest and therapy, and the pain remains severe enough to interfere with work or recreation, the next diagnostic test should be a cervical MRI scan to evaluate the cervical discs. Usually the study is normal or shows mild cervical disc dehydration with disc bulging. Neck pain from cervical disc dehydration can best be treated by cervical traction. Minor cervical disc bulging presenting with chronic pain, with a normal neurologic exam, is rarely sufficient indication for surgery. At this point, it is best to get the opinion of a neurosurgeon.
II. NONTRAUMATIC NECK PAIN OF ARTHRITIC ORIGIN
A. Introduction. Neck pain from degenerative arthritis of the neck is of epidemic proportion (60% to 80%) in the elderly population.
B. Etiology. Degenerative arthritis of the cervical spine occasionally manifests itself as early as the third decade of life but is much more common with increasing age. Disc dehydration and disc space narrowing with osteophyte formation is a process that occurs naturally with age. Facet arthritis also occurs. Small nerve fibers innervating the disc and facet can be involved leading to neck pain. Dural impingement by osteophytes can also produce neck pain—especially with extension or lateral gaze.
C. Evaluation.
1. History and physical examination. Nontraumatic neck pain in the over 40 age group is most often secondary to cervical degenerative arthritis. The pain is gradual in onset and initially intermittent and then becomes more constant. There can be associated occipital headache and interscapular pain. Motion, especially extension or lateral gaze, can aggravate the pain.
2. Radiographs. X-rays show narrowing of disc spaces with bone spur formation. At least 70% of the populations over the age of 65 have significant changes of degenerative arthritis. Regardless of how bad the X-rays look, if the patient is neurologically normal, MRI or surgery is not absolutely indicated.
D. Referral.
1. Medication. (Same as for traumatic neck pain.)
2. Physical therapy. Heat, ultrasound, massage, and TENS unit therapy can help.
3. Pain clinic. Trigger point injections can help.
4. Alternative therapies. Although chiropractors can help many people, we cannot advocate manipulation of the neck when obvious bone spurs exist. Neurologic catastrophes and lawsuits have occurred. Patients can seek chiropractic care at their own risk. Recently, magnets have become popular in relieving arthritic complaints with some scientific credence. Finally, oral glucosamine has been shown somewhat effective against arthritis, although its effect on cervical spondylosis remains to be determined.
5. Spine specialists. In the majority of patients with neck pain and no arm pain, surgery is not indicated. The removal of large osteophytes ventral to the spinal cord can improve severe neck pain, occipital headache, and actually improve the range of motion. Only an experienced spinal surgeon should make this decision based on a CT scan/MRI scan and repetitive physical exams over a period of time.
III. NECK PAIN WITH ARM PAIN (RADICULOPATHY) FROM SOFT CERVICAL DISC BULGES/HERNIATIONS
A. Etiology. In the under-50 age group, the most common cause will be a single-level soft cervical disc. The concept of a soft cervical disc means either an eccentric disc bulge or a free fragment herniation compressing a root. A disc consists of an inner water-laden mucoid nuclear material and an outer fibrous annulus. The annulus can fissure, allowing the nucleus either to bulge or to herniate out. There is no osteophyte involved in the compression. The posterior longitudinal ligament extends beneath the entire spinal cord, protecting the cord from disc herniation, and so a disc herniation primarily projects laterally into the foramen, compressing the nerve only. In rare cases, sufficient force, such as in trauma, can lead to a large disc herniation, causing an acute myelopathy.
B. Anatomy. A disc is named by the bordering vertebral bodies. Thus, the disc between vertebral bodies C5 and C6 is named the C5–C6 disc. The nerve root whose number corresponds to that of a given vertebral body exits above that body’s pedicle. Thus a C5–C6 disc compresses the C6 nerve root.
C. Evaluation.
1. History. In the classic story, there is intermittent neck pain and then severe neck pain, and arm pain develop. Rarely is this condition traumatic in origin. The pain radiates down the shoulder and into the arm. There are some dermatomal patterns of radiation that can help discern the level of herniation. Patients may complain of various combinations of suboccipital headache, interscapular pain, numbness, tingling, and weakness. The pain often awakens the patient from sleep.
2. Physical exam.
a. Neck exam. There is posterior tenderness, especially tenderness at the spinous process near the level of involvement and paracervical tenderness. Painful limitation of motion with extension and lateral gaze to the side of arm pain is classic.
b. Arm exam.
(1) C5 radiculopathy (C4–C5 disc herniation) presents with pain and numbness radiating to the shoulder along with a weak deltoid muscle (shoulder abduction). Simultaneous testing of both deltoid muscles by compression on the outstretched upper arms detects minor weakness (Table 22.1). There is no true muscle stretch reflex to test.
(2) C6 radiculopathy (C5–C6 disc herniation). C5–C6 disc herniation is the second most common cervical disc herniation. Pain and numbness radiate across the top of the neck and along the biceps to the lateral aspect of the forearm, and dorsal thumb and index finger. Numbness is usually more distal. A weak biceps, a reduced biceps reflex and weak wrist extension are observed.
(3) C7 radiculopathy (C6–C7 disc herniation). This is the most common disc herniation. Pain radiates across the top of the neck, across the triceps, and down the posterolateral forearm to the middle finger. Numbness again is more distal. A weak triceps and reduced triceps reflex are observed.
(4) C8 radiculopathy (C7–T1 disc herniation) is very uncommon. Pain and numbness radiate across the neck and down the arm to the small finger and ring finger. Wrist flexion and the intrinsic muscles of the hand are weak.
3. Radiographic evaluation.
a. Plain X-rays provide very little help. They may show slight narrowing of the disc space involved and loss of lordosis.
b. An MRI scan without contrast is the study of choice for demonstrating a cervical disc herniation (Fig. 22.1).
4. Electromyogram (EMG) and nerve conduction velocity studies (NCVs). An EMG for a single-level disc herniation with a radiculopathy is not absolutely necessary. It can help when other disorders, such as amyotrophic lateral sclerosis, carpal tunnel syndrome, and brachial plexopathy, need to be ruled out.
TABLE 22.1 Motor Strength Classification (0 to 5 Scale)
0, no movement
1, flicker of movement
2, able to move but not against gravity
3, able to move against gravity but offers no resistance
4, offers resistance but able to overcome or easy fatigue
5, normal
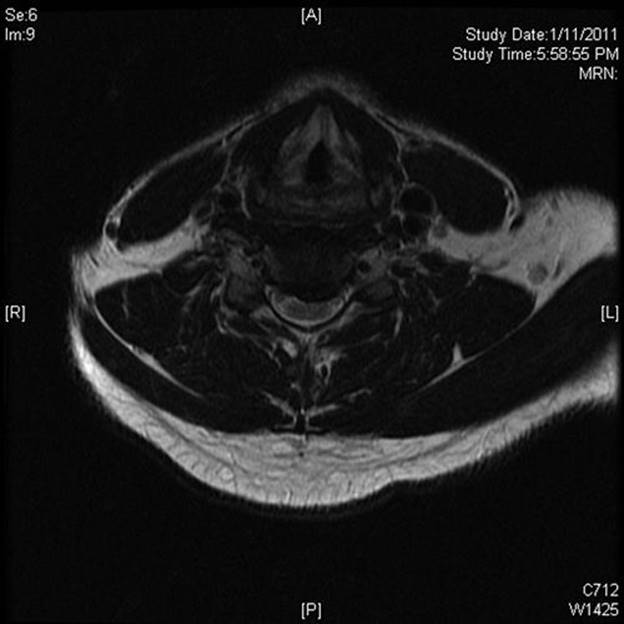
FIGURE 22.1 Axial T2-weighted MRI demonstrating a large eccentric cervical disc protrusion (C5–C6) causing impingement on the ventral aspect of the spinal cord and foraminal impingement.
D. Referral.
1. Physical therapy. After diagnosis by MRI, a patient with a motor strength rating of 4/5 or more (Table 22.1) can be referred for cervical traction, heat, ultrasound, massage, and a soft collar. Initially, cervical traction should be done by a physical therapist. Inform the therapist that if traction is tolerated; the patient is to be instructed in home cervical traction at 10 lb for half-an-hour every night. Approximately 60% to 80% of soft disc herniations improve to the point of resolution of the radiculopathy with traction alone within 4 to 6 weeks. Not every patient can tolerate traction.
2. Medication. A trial of 4-mg self-weaning methylprednisolone (Medrol) dose pack can be used early in the treatment prior to nonsteroidals with some success. Other medicines were previously discussed in the section on traumatic neck pain.
3. Time-off from work. Desk-type workers with mild to moderate neck/arm pain can work, and most ambitious people are able to function. Heavy laborers may benefit from light duty or 1 to 4 weeks off work. Beware of patients who exhibit symptom magnification and functional overlay for purposes of secondary gain (worker’s compensation and litigation). They have the tendency to abuse time-off work. In these scenarios, early referral to a physical medicine and rehabilitation specialist who can scientifically assess for malingering may be helpful.
4. Spine specialist. In any patient with three-fifth strength or worse, immediate referral to a spine surgeon is indicated. The longer a root is compressed with severe weakness, the less likely strength will return to normal. If the strength remains four-fifth or better but pain persists after 3 to 6 weeks of traction, then referral to a spine surgeon is also indicated. A well-trained spine surgeon should achieve improvement of arm pain and weakness in 90% to 95% of soft cervical disc herniations.
IV. NECK PAIN WITH ARM PAIN FROM BONE SPURS (HARD DISC, CERVICAL SPONDYLOSIS)
A. Introduction. The combination of neck pain and arm pain in cervical spondylosis is also of epidemic proportions in the elderly population.
B. Etiology. Disc dehydration and narrowing leads to bone spur formation at the margins of the vertebral body. The spurs can project into the foramen or canal, compressing the nerve root or the spinal cord, or both. In addition, facet arthritis with resultant hypertrophy and ligamentous hypertrophy also narrow the spinal canal and neural foramens. With progressive age, more than one disc space is usually involved. The center of the process usually extends from C4 to C7.
C. Evaluation.
1. History. This condition occurs primarily in patients older than soft cervical disc herniation patients, although the two groups overlap. About 90% of patients have gradual onset of neck pain with progression to neck and arm pain. The pain radiates down the shoulder and into the arm. There are some dermatomal patterns of radiation that can help discern the level of root compression. Various complaints of suboccipital headache, interscapular pain, numbness, tingling, and weakness may also be present. The pain often wakes the patient up from sleep. About 10% of patients have asymptomatic degenerative arthritis, and then symptoms of neck pain/arm pain are often precipitated by hyperextension/flexion injuries from trauma (motor vehicle accidents.) A large percentage have multiple disc spaces involved, making it more difficult to determine which level or levels caused the radiculopathy.
2. Physical examination.
a. Neck examination. There is posterior tenderness, especially tenderness at the spinous process near the level of involvement and paracervical tenderness. Painful limitation of motion with extension and lateral gaze to the side of arm pain is classic.
b. Arm examination (see Table 22.1) same as discussed in soft cervical disc section.
c. Leg examination (Table 22.2). Gait is usually normal even in the face of significant radiographic evidence of spinal cord compression. Occasionally, myelopathy is present. Early on, the gait is normal in the face of increased muscle stretch reflexes and Babinski’s sign. With more severe and prolonged compression, one can observe spastic gait with bowel and bladder problems. In the most severe cases, the patient requires a cane or a walker. Rarely is it allowed to progress to wheel chair dependency.
3. Radiographs.
a. Plain X-rays show disc space narrowing with osteophyte (bone spur) formation. Oblique films can exhibit neuroforaminal narrowing.
TABLE 22.2 Nurick Classification
|
Grade |
Characteristic |
|
1 |
Signs of spinal cord disease but normal gait |
|
2 |
Slight gait abnormality not preventing full time employment |
|
3 |
Gait abnormality severe enough to prevent employment or housework. Still able to ambulate independently |
|
4 |
Requires a walker or someone else’s help to ambulate |
|
5 |
Wheelchair bound |
b. MRI scan (Fig. 22.2). It is excellent for demonstrating nerve-root compression and cord compression from bone spurs. It does not provide as much detail about bone anatomy as the CT scan.
c. CT scan (Fig. 22.3A, B). It shows better bone detail than MRI, but is not as good at showing the neural structures. The two studies together are ideal for this group of patients, but this is obviously not cost effective, so MRI is the first choice.
4. EMG and NCVs. An EMG can be helpful in discerning which roots are most involved in patients with multi-level spondylosis.
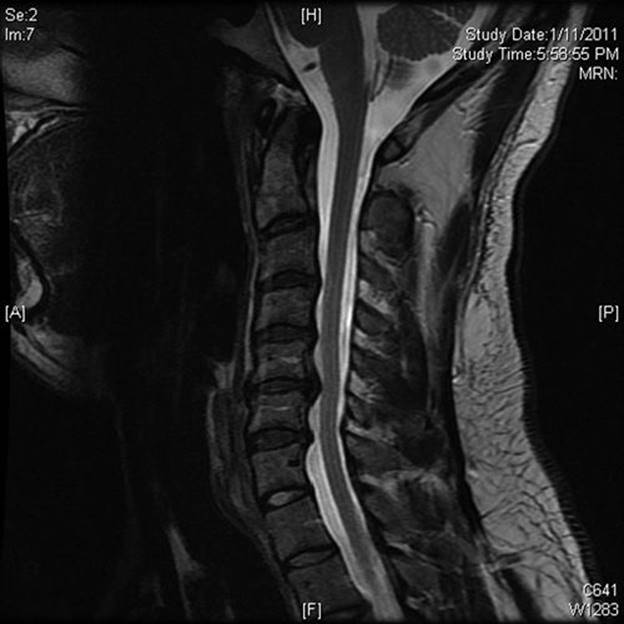
FIGURE 22.2 Sagittal MRI of the cervical spine demonstrating multiple-level spondylosis.
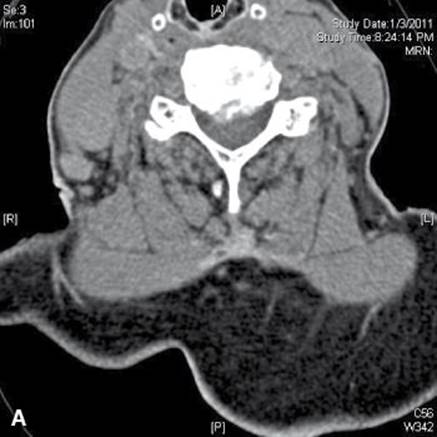
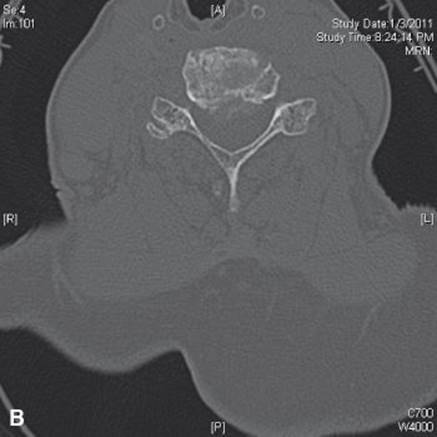
FIGURE 22.3 Axial CT with soft tissue (A) and bone windows (B) demonstrating moderate to severe central canal stenosis secondary to an eccentric disc protrusion (C5–C6) as well as osteophyte with foraminal stenosis.
D. Referral.
Medication. As discussed in previous medication sections.
1. Soft cervical collar.
2. Physical therapy. Heat, ultrasound, massage, traction, and TENS can reduce the symptoms. Approximately 20% of the radiculopathies (arm pain/strength) can be successfully improved with medicine and therapy alone for many years. The majority of patients have some pain with persistent mild weakness (if any weakness is present). Rarely does myelopathy develop in this group of patients.
3. Spine specialist. Surgery for cervical spondylotic radiculopathy is almost always elective. Results of surgery are much better for single-level disease than for multi-level disease, especially for neck pain. Arm motor strength of three-fifth or worse and any evidence for myelopathy is an indication for immediate referral to a spine surgeon. The anterior approach is superior to the posterior approach if bone spurs project under the entire spinal cord. Surgery helps the radiculopathy in 90% to 95% of both single-level disease and multi-level disease patients, but neck pain improves in only 70% to 75% of multi-level disease patients. Complete relief of radicular pain occurs in approximately 60% to 80% of cases. There is no age cutoff for surgery as long as patient is in reasonable medical condition. The elderly tolerate surgery very well with minimal morbidity. If a myelopathy is present with gait abnormality and an aggressive decompression is performed, an improvement of one grade on Nurick’s scale (see Table 22.2) can be expected in 70% to 80% of patients. Duration of symptoms is very important for patients with gait problems. Thus early referral is indicated.
V. NECK PAIN WITH/WITHOUT ARM PAIN DUE TO METASTATIC CANCER OF THE CERVICAL SPINE
A. Introduction. As patients live longer with various malignancies, the number of patients who present with spine metastases also increases. The tumors that most commonly involve the spine are lung cancer, breast cancer, prostate cancer, lymphomas, and multiple myeloma. As many as 20% of these tumors will develop symptomatic spinal involvement. In approximately 10% of patients, metastatic spinal involvement will be the mode of presentation with no known primary tumor.
B. Evaluation.
1. History and physical examination. Both primary and metastatic tumors of the spine initially present with pain that is often worse at night. The pain continues to worsen over a very short period, and then neurologic symptoms, such as radiculopathy and myelopathy, develop fairly quickly. It is best to make the diagnosis when neurologic symptoms are minimal.
2. Radiographs.
a. Plain X-rays can show destruction of the vertebral bodies and pedicles (Fig. 22.4). Pathologic compression fractures and lytic pedicles are very common. The sensitivity of plain X-rays is approximately 60%.
b. Bone scans are very sensitive—approaching 100%—in showing spine metastases, including asymptomatic areas with no destruction.
c. MRI scans are ideal for delineating canal involvement, cord compression, and surgical feasibility.
C. Referral.
1. Radiation therapy. Diffuse disease involving large amounts of the spine is treated primarily with steroids and radiation therapy. Radiation is usually reserved for the symptomatic areas only. Dexamethasone 2 to 20 mg P.O. every 6 hours can be quite helpful in improving pain and neurologic symptoms.
2. Surgery. Early referral to a spine surgeon is warranted following diagnosis regardless of the neurologic exam. If surgery is indicated, it is often best to perform it prior to radiation therapy, because this reduces the wound complication rate. In the face of a cervical myelopathy resulting from diffuse canal involvement and cord compression, a laminectomy can be performed. Patients with lung cancer do very poorly and it is hard to justify surgery scientifically for metastatic lung cancer unless there is no primary disease the spine disease is the only systemic metastasis. Other tumors do better, but a good rule is 30% to 50% of all tumors are improved by laminectomy with a 10% mortality rate. Isolated vertebral body disease can be resected from an anterior approach—especially in well-controlled breast cancer, prostate cancer, lymphoma, and renal cell cancer with excellent long-term results that are superior to radiation alone.
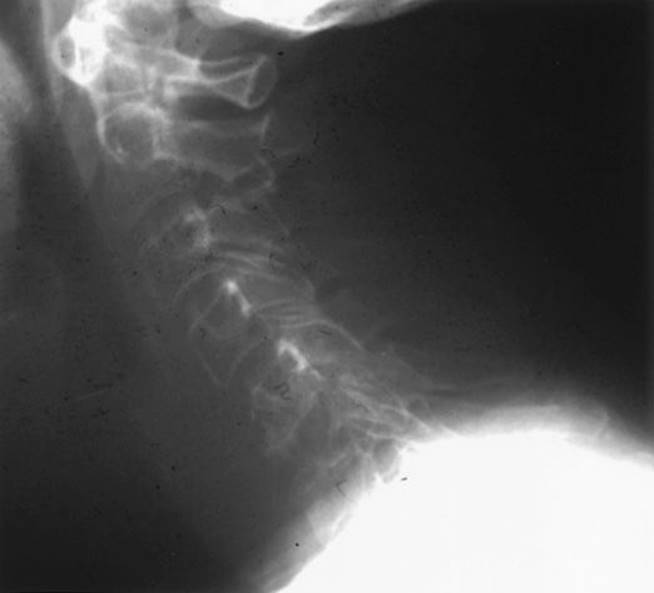
FIGURE 22.4 Lateral radiograph demonstrating lytic destruction of the C6 vertebral body.
VI. MISCELLANEOUS NECK PAIN WITH/WITHOUT ARM PAIN
A. Rheumatoid arthritis.
1. Etiology. Rheumatoid arthritis can affect the C1–C2 articulation leading to erosion of the odontoid process and transverse atlantal ligament, which leads to C1–C2 instability and cord compression from the developing panus.
2. Evaluation.
a. History and physical examination. Severe neck pain is usually followed by arm pain and a progressive myelopathy.
b. Radiographs. Plain X-rays and MRI scans are best for showing erosion of the odontoid process with subsequent instability (Fig. 22.5).
3. Referral and therapy. Place a soft collar and refer immediately to a spine surgeon. Posterior C1–C2 fusion with transarticular screws is ideal for the problem; occasionally an anterior transoral odontoidectomy is required. These treatments are not without risk and must be individualized.
B. Discitis/osteomyelitis.
1. Introduction. Bacterial discitis/osteomyelitis is extremely uncommon in the cervical spine and fever may not be present.
2. Evaluation.
a. History and physical examination. There may be a prior history of skin infection, urinary tract infection, or pulmonary infection. Iatrogenic discitis/osteomyelitis complicating cervical spine surgery is known to occur. Perhaps the most common cause in urban settings is a history of intravenous drug abuse. Progressive neck pain with a rapidly progressive myelopathy is the usual presentation.
b. Radiographs. Plain X-rays show disc space collapse with erosion of the bordering vertebral bodies. MRI shows epidural spinal cord compression from kyphosis or epidural abscess.
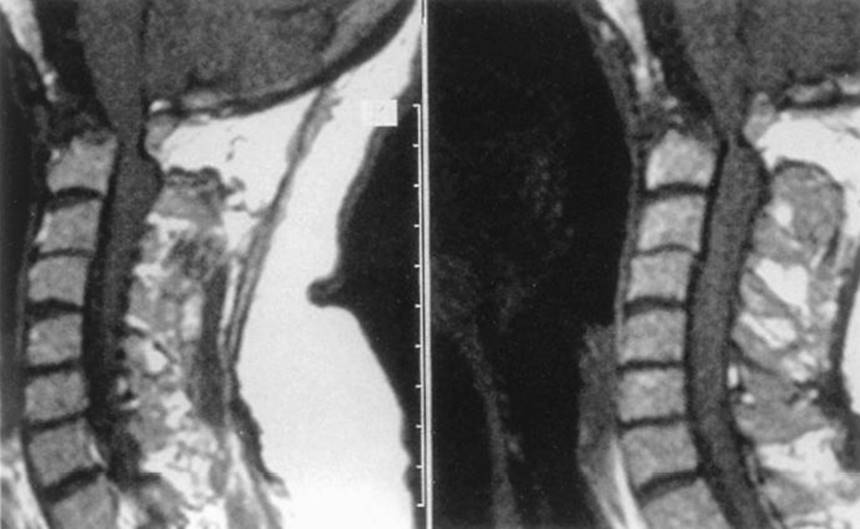
FIGURE 22.5 Left and right: Sagittal MRI scans in rheumatoid arthritis demonstrating destruction of the dens with compression of the medulla and spinal cord at the cranio-cervical junction.
3. Referral. The patient should be immediately referred to either a spine specialist or an infectious disease specialist. An immediate radiology-directed needle biopsy/culture or open biopsy culture, and administration of intravenous bactericidal antibiotics for at least 6 weeks, are indicated. Surgical debridement and decompression are performed for severe kyphosis and neurologic problems.
![]()
Recommended Readings
Bracken M, Shephard M, Collins W, et al. Methylprednisolone or naloxone treatment after acute spinal cord injury: 1 year follow up data. Results of the second national acute spinal cord injury study. J Neurosurg. 1992;76:23–31.
DePalma A, Rothman R, Levitt R, et al. The natural history of severe cervical disc degeneration. Acta Orthop Scand. 1972;43:392–396.
Melhem E. Technical challenges in MR imaging of the cervical spine and cord. Magn Reson Imaging Clin N Am. 2000;8:435–452.
Modic M, Masaryk T, Ross J, eds. Magnetic Resonance Imaging of the Spine. Chicago, IL: Year Book Medical Publishers; 1989.
Patchell R, Tibbs P, Regine W, et al: Direct decompressive surgical resection in the treatment of spinal cord compression caused by metastatic cancer: a randomized trial. Lancet. 2005;366:643–648.
Pellicci P, Ranawat C, Tsairis P, et al. A prospective study of the progression of rheumatoid arthritis of the cervical spine. J Bone Joint Surg Am. 1981;63:342–350.
Ropper A, Samuels M. Adams and Victor’s Principles of Neurology. 9th ed. New York, NY: McGraw Hill Inc; 2009.
Rothman R, Simeone F, eds. The Spine. Vol 1 & 2. Philadelphia, PA: WB Saunders & Co; 1992.
Shapiro S. Banked fibula, locking cervical plate following anterior cervical discectomy. J Neurosurg. 1996;84:161–165.
Shapiro S. Spinal instrumentation with a low complication rate. Surg Neurol. 1997;48:566–574.
Wilkins R, Rengachary S, eds. Neurosurgery. Vol 1–3. New York, NY: McGraw-Hill Book Co; 1996.
Wong D, Fornasier V, MacNab I. Spinal metastases: the obvious, the occult and the imposters. Spine. 1990;15:1–4.